Hair loss in women (female hair loss or female pattern hair loss) is the excessive thinning or shedding of hair from the scalp that exceeds normal daily hair loss. Anything beyond the signal is an underlying issue, while it is common for women to lose 50 to 100 strands per day. Understanding the condition is important because early detection and management help prevent permanent thinning and improve hair regrowth outcomes. Female hair loss affects appearance and causes significant emotional and psychological distress. Women report reduced self-esteem, social anxiety, and depression related to their changing appearance. The physical signs, such as a widening part or thinning at the crown, appear gradually, making it easy to miss early warning signs. Recognizing the first signs of hair thinning is key to starting treatment promptly. Hair loss in women is a normal but manageable condition, though distressing. Women reduce further loss and stimulate regrowth with proper diagnosis and treatment. The guide provides a comprehensive overview of the different types of hair loss, common symptoms, causes of hair loss in women, and available hair loss treatment for women.
Female pattern hair loss (FPHL) affects up to 40 percent of women by age 50, according to research published in the Journal of Investigative Dermatology, and the risk increases with age and hormonal changes. Common causes include genetic predisposition (androgenetic alopecia), stress-induced shedding (telogen effluvium), hormonal imbalances (thyroid disorders or PCOS), autoimmune conditions (alopecia areata, and nutritional deficiencies). Each cause has distinct patterns and responses to treatment. Effective hair loss treatment for women depends on the underlying cause. Topical minoxidil, oral anti-androgens such as spironolactone, low-level laser therapy, platelet-rich plasma (PRP), and lifestyle change all play a role. Early intervention, especially at the stage of first signs of hair thinning, offers the best chance for successful regrowth and long-term control. Female hair loss is a complex condition influenced by multiple factors. Understanding the different types, identifying causes, and exploring appropriate treatments, women take proactive steps to protect their hair and restore confidence.
How Common Is Sudden Hair Loss in Women?
Sudden hair loss in women is common in adults between the ages of 30 and 60. About 4 in 10 women experience visible hair loss by age 50, and around 1 in 10 adult women deal with sudden or rapid hair loss female at some point, according to AAD, 2022. Specific causes (telogen effluvium) affect 10% to 20% of women (NIH, 2021), while about 2% of all women develop alopecia areata, according to NAAF, 2022. It shows that women’s hair loss is not rare and appears during adulthood rather than childhood.
Hair loss is more common in adult women than in girls. Adults face more internal triggers like hormone shifts during menopause, thyroid issues, chronic stress, or nutrient deficiencies. They are more likely to have external triggers such as tight hairstyles, heat tools, and chemical treatments. Children experience hair loss due to rare autoimmune issues or scalp infections, which are much less frequent.
The age range for sudden hair loss in women tends to start in the 30s and peak around midlife. Events like pregnancy, illness, emotional stress, or surgery trigger rapid shedding. Four out of ten women show signs of hair loss with age, which makes women’s hair loss a widespread and age-related condition.
What Are the Signs and Symptoms of Hair Loss in Women?
The Signs and Symptoms of Hair Loss in Women are listed below.
- Thinning hair on top of the head: The most common sign, especially with female pattern hair loss. Hair density reduces at the crown or mid-scalp, leading to less volume and a flatter appearance.
- Widening part: The part line becomes noticeably wider under direct lighting as the hair thins. It is the first visible change women notice.
- Receding hairline: Women experience a slow retraction of the hairline, although less common in women near the temples.
- Increased hair shedding: Clumps of hair come out while combing, showering, or even resting on pillows. It is different from normal daily shedding and indicates an underlying issue.
- Patchy bald spots: Some types of hair loss, like alopecia areata, cause sudden round or oval patches of total hair loss. The areas appear smooth and skin-colored.
- Slow hair growth: Hair grows back thinner, shorter, or slower than usual. Regrowth does not keep up with the rate of loss.
- Scalp visibility: The scalp becomes more visible through the hair, under natural or bright lighting. A sign of overall hair density reduction.
- Itchy or irritated scalp: Scalp discomfort, such as itching, tingling, or burning, occurs before or during hair loss if there’s an inflammatory or autoimmune cause.
What Are the Early Symptoms of Hair Loss in Women?
The early symptoms of hair loss in women are listed below.
- Widening Part Line: One of the first signs is a gradually widening part, especially along the crown. It is a localized thinning specific to female pattern baldness, compared to general shedding.
- Thinner Ponytail: Women notice their ponytail feels smaller or thinner. The reduction in volume is progressive and consistent, unlike seasonal shedding.
- Increased Hair on Pillow or Shower Drain: More strands appear on pillows, brushes, or shower drains. The shedding differs from regular loss due to its persistent and increasing frequency.
- Scalp Visibility: The scalp becomes more visible, especially under bright light. It occurs at the center and crown of the head, unlike receding hairlines in men.
- Short, Broken Hairs: Hair strands become shorter and weaker, indicating miniaturization. It is a distinct sign of follicle shrinkage, unlike breakage from styling.
- Slower Hair Growth: Hair takes longer to grow back after a cut. It means that there has been a disruption in the hair renewal cycle compared to healthy hair renewal.
- Loss of Hair Density at the Crown: Hair becomes less dense on the top, but remains full on the sides. The pattern is typical of female pattern baldness, not telogen effluvium.
- Itchy or Sensitive Scalp: Women report itchiness or tenderness where thinning begins. It indicates inflammation at the follicles, but not always present.
What Are the Late Signs of Hair Loss in Women?
The late signs of hair loss in women are listed below.
- Large Bald Spots: Bald spots develop in the crown and top areas, where thinning is most severe. The spots become larger and more noticeable, indicating significant follicle loss, unlike early-stage thinning.
- Widened Scalp Visibility: The scalp becomes clearly visible across the entire top of the head. The visibility of the scalp becomes more diffuse and widespread in comparison to earlier stages, signaling advanced hair loss.
- Receding Hairline: A receding hairline is a distinct feature of severe female hair loss, where the hairline begins to pull back around the forehead, similar to male pattern baldness. It differs from the earlier, more diffuse thinning that affects the crown and part lines.
- Sparse Areas at the Crown: There are large areas of sparse hair around the crown, which are easily noticeable in bright light. It contrasts with earlier stages, where thinning is more concentrated and less noticeable.
- Visible Scalp Texture: The texture of the scalp becomes rough or uneven due to widened follicles. The sign indicates advanced miniaturization of hair follicles and is distinctly more severe than the earlier thinning at the part.
- Total Loss of Volume: There is a complete loss of volume, and the hair appears flat or lifeless even when styled. It is a stark contrast to early signs like thinning ponytails, where some volume still remains.
Does Extreme Hair Falling Out Mean Symptoms of Hair Loss in Women?
Yes, extreme hair falling out is a symptom of hair loss in women. Hair falling out in women’s experience goes beyond the normal 50–100 strands per day. It signals an underlying issue such as telogen effluvium, iron deficiency, thyroid problems, or hormonal changes (PCOS or menopause). Extreme shedding shows up suddenly and results in handfuls of hair on brushes, pillows, or shower drains. Shedding differs from gradual thinning and is temporary or chronic depending on the cause. Stress-related telogen effluvium triggers large amounts of hair to enter the resting phase, shedding all at once after a few months. Hair falling out women notice reduced density, visible scalp, or difficulty styling due to volume loss. Clinical signs that the body is reacting to internal or external stressors, and early intervention is key to reversing or managing the condition.
Does a Sudden Bald Spot Mean Hair Loss in Women?
Yes, a sudden bald spot means hair loss in women. Losing large amounts of hair suddenly is not normal and points to a medical or hormonal issue. A woman experiences rapid hair loss due to stress, thyroid disorders, nutrient deficiencies, or autoimmune conditions (alopecia areata). Sudden bald spot on head woman cases are linked to alopecia areata, where the immune system attacks hair follicles. It results in round, smooth patches of total hair loss that appear overnight. Rapid hair loss female caused by telogen effluvium begins 2 to 3 months after a trigger (illness, childbirth, or emotional shock). Extreme shedding signals a disruption in the normal hair growth cycle. It leads to long-term thinning or patchy loss when treated, making early evaluation important.
Where on the Scalp Does Hair Thinning in Women First Occur?
Hair thinning in women occurs in the crown or the midline part of the scalp. Women notice thinning where they part their hair, which gradually becomes wider. The characteristics of female pattern hair loss (FPHL), medically known as androgenetic alopecia, affect the central scalp region first while preserving the frontal hairline. The areas are more sensitive to androgens, dihydrotestosterone (DHT), which miniaturize hair follicles. Women predisposed to FPHL tend to have hair follicles in the crown region that progressively shrink, producing thinner and shorter hair shafts over time.
FPHL presents as a diffuse reduction in hair density over the crown and frontal scalp with retention of the frontal hairline, according to a review published in the “Journal of Clinical and Diagnostic Research” dated 2014. The Ludwig Scale, used to classify female pattern hair loss, confirms the common pattern, showing stages of increasing thinning at the center scalp while the front remains intact. A study by Birch et al. (2001) in the British Journal of Dermatology found that 38% of women over 70 showed evidence of female pattern hair loss, starting primarily at the central part. It supports the observation that thinning begins along the mid-scalp and spreads outward as the condition progresses. Early detection of central scalp thinning is critical for diagnosis and treatment to prevent further hair miniaturization and loss.
What Are the Different Hair Loss Stages in Women?
The different hair loss stages in women are listed below.
- Stage I: Stage I involves mild thinning concentrated at the central part of the scalp. The part line begins to widen, but the frontal hairline remains preserved. Hair density appears normal under standard lighting conditions. Stage I, the first classification of the Ludwig Scale, is the most responsive stage to treatment.
- Stage II: Stage II is marked by moderate thinning that extends outward from the center of the scalp. The part line becomes wider, the scalp is more exposed, and overall hair volume decreases. Styling becomes more difficult due to limited coverage.
- Stage III: Stage III represents severe thinning or near baldness at the crown and top of the scalp. Hair density is visibly low, and the scalp is easily seen, even in low light. The frontal hairline remains, but the crown area is exposed and nearly bare. The stage reflects advanced Female Pattern Hair Loss and shows limited response to non-surgical treatments.
What Are the Causes and Reasons of Hair Loss in Women?
The causes and reasons of hair loss in women include a mix of hormonal, genetic, autoimmune, and environmental factors. The most frequent cause of hair loss in women is hormonal imbalance, including shifts from pregnancy, menopause, or thyroid issues. Less common alopecia causes in females include autoimmune conditions like alopecia areata and inherited disorders. Female pattern hair loss, or androgenetic alopecia, is a leading cause in females, showing gradual thinning at the crown. Alopecia areata leads to sudden, round bald patches due to the immune system’s attack. Androgenetic alopecia progresses slowly and affects more women, while alopecia areata appears abruptly and is less predictable.
The causes and reasons for hair loss in women are listed below.
- Hormonal changes: Pregnancy, menopause, or thyroid dysfunction disrupt the hair cycle. An estrogen drop after childbirth leads to telogen effluvium.
- Genetics (Androgenetic alopecia): The most common cause of hair thinning in women, inherited. It affects the crown and part line, progressing gradually.
- Stress or trauma: Physical or emotional stress causes sudden shedding (telogen effluvium). Hair regrows after 3 to 6 months if the stressor is removed.
- Autoimmune disorders (Alopecia areata): The immune system attacks hair follicles, causing round bald spots. It is unpredictable and varies in severity.
- Nutritional deficiencies: Lack of iron, vitamin D, or protein weakens hair structure and growth. It is common in restrictive diets or absorption disorders.
- Medical treatments: Chemotherapy, radiation, and certain medications (antidepressants, beta-blockers) trigger widespread hair loss.
- Hair styling and damage: Tight hairstyles, heat tools, and chemical treatments cause traction alopecia. Common in women who alter hair texture or color.
- Scalp infections or diseases: Fungal infections (tinea capitis) lead to patchy, inflamed scalp hair loss. Conditions like seborrheic dermatitis or psoriasis disrupt follicles.
What Are the Most Common Causes of Hair Loss in Women?
The most common cause of hair loss in women is androgenetic alopecia (female pattern hair loss). The condition causes gradual thinning of hair at the crown and along the part line, due to genetics and hormonal sensitivity to androgens like DHT (dihydrotestosterone). It begins after puberty and becomes more noticeable with age. Androgenetic alopecia affects up to 40% of women by age 50, according to the Journal of Investigative Dermatology (2003). Over 38% of women over age 70 showed visible signs of the condition, according to the study by Birch et al. (2001). It occurs when predisposed hair follicles shrink over time and produce thinner, shorter hairs.
Hair loss in women varies based on age, genetics, hormonal health, ethnicity, and underlying medical conditions. Thinning increases after menopause due to reduced estrogen, a hormone that helps protect hair follicles. Genetics plays a major role, as women with a family history of pattern baldness are more likely to develop androgenetic alopecia. Hormonal conditions such as polycystic ovary syndrome (PCOS), thyroid disorders, and postpartum hormone shifts trigger or worsen shedding. Ethnic and demographic factors influence hair loss patterns. Traction alopecia is more common in African-American women due to certain hairstyling practices. Underlying health issues (iron deficiency, autoimmune diseases, and stress-related telogen effluvium) contribute to temporary or chronic hair loss, although the causes are less persistent than genetically driven thinning.
Is Stress the Most Common Reason of Hair Fall in Females?
No, stress is not the most common reason for hair fall in females. The most frequent cause of hair fall in women is androgenetic alopecia, known as female pattern hair loss. The condition is caused by genetics and hormonal sensitivity. Stress is a recognized trigger of hair loss in cases of telogen effluvium, but it is not the leading cause in long-term cases.
Stress-related shedding starts two to three months after a significant physical or emotional event. Stress results in temporary thinning across the scalp. It makes it one of several hair fall reasons in females, but not the most dominant one. Hair regrows once the stress is managed.
Androgenetic alopecia causes progressive and long-term thinning. Androgenetic alopecia affects the part line and crown and impacts up to 40% of women by age 50. The top cause of hair fall in women is genetic and hormonal in nature, while stress is a common trigger. Genetics, aging, hormonal imbalance, and health issues are more consistent reasons for hair fall in women over time.
What Are the Rare Causes of Female Hair Loss?
The rare causes of female hair loss include scarring alopecias, lupus, lichen planopilaris, trichotillomania, and certain inherited genetic syndromes. The conditions account for a small percentage of hair loss cases and are considered rare due to their low prevalence in the general population. Scarring alopecias, such as lichen planopilaris and central centrifugal cicatricial alopecia (CCCA), involve permanent destruction of hair follicles due to inflammation or autoimmune attack.
The conditions affect fewer than 3% to 5% of women with hair loss, according to data from the Journal of the American Academy of Dermatology (JAAD) dated 2002. The conditions are less diagnosed and require a biopsy to confirm because the condition does not follow common patterns like diffuse thinning or widening of the part seen in androgenetic alopecia.
Rare causes of female hair loss have distinct features and are influenced by personal factors. Scarring alopecia causes permanent hair loss due to follicle destruction, with a smooth, shiny, and inflamed scalp. Lupus erythematosus leads to patchy hair loss and scalp lesions, sometimes affecting body hair. Lichen planopilaris causes perifollicular scaling and scarring. Trichotillomania is a compulsive hair-pulling disorder linked to mental health, while inherited syndromes like hypotrichosis cause abnormal or absent hair from childhood.
The rare causes vary with age, gender, genetics, and health. Autoimmune types (lupus and lichen planopilaris) are more common in middle-aged women. Trichotillomania is seen in adolescent females. CCCA is more frequent in women of African descent due to hair care practices and genetic risk. Inherited disorders are diagnosed early in life and remain extremely rare. Women with autoimmune or inflammatory diseases face a higher risk of scarring alopecia.
What Are the Lifestyle Factors that Can Cause Hair Loss in Females?
The Lifestyle Factors that can Cause Hair Loss in Females are listed below.
- Nutritional deficiencies: Diets low in iron, vitamin D, protein, or biotin weaken hair structure and reduce growth. Females with diffuse hair loss had lower serum ferritin and vitamin D levels compared to healthy controls, according to a study titled “Journal of Clinical and Diagnostic Research” dated 2016.
- Chronic stress: High stress levels shift hair follicles into the resting (telogen) phase, leading to shedding. Elevated cortisol levels and psychological stress were directly linked to increased hair loss in women, according to a study published in “PLoS One” dated 2021.
- Crash dieting or eating disorders: Severe calorie restriction causes acute nutrient loss and disrupts the hair cycle. Rapid weight loss and eating disorders like anorexia nervosa were associated with telogen effluvium in women, according to an article titled “American Journal of Clinical Dermatology” dated 2010.
- Poor sleep habits: Inadequate sleep alters hormone levels melatonin and cortisol, which affect hair growth. Melatonin contributes to hair follicle growth regulation, and its disruption through sleep loss impairs the cycle, according to research published in “International Journal of Molecular Sciences” dated 2020.
- Smoking: Nicotine reduces blood circulation to the scalp, increasing oxidative stress and inflammation in follicles. A strong association between smoking and androgenetic alopecia in women. Smokers have moderate to severe hair loss, according to a study in “Dermatology” dated 2003,.
- Excessive alcohol consumption: Alcohol depletes zinc and B-complex vitamins needed for healthy follicles. Alcohol misuse is linked to nutritional deficiencies and liver dysfunction that impair hair growth, according to a review in “Skin Appendage Disorders” in 2017.
- Tight hairstyles or overstyling: Continuous tension from braids, weaves, or ponytails damages hair follicles over time. Traction alopecia is a common cause of hair loss in African-American women due to styling practices, according to a clinical review in “American Academy of Dermatology” dated 2007.
- Lack of scalp hygiene: Product buildup and sebum block follicles and trigger inflammation or infection. Poor scalp hygiene correlated with increased incidence of seborrheic dermatitis and diffuse hair loss, according to a study titled “Skin Research and Technology” in 2014.
What Types of Medications Can Cause Hair Loss in Women?
The types of medications that can cause hair loss in women are listed below.
- Chemotherapy drugs: Directly attack rapidly dividing cells, including hair follicles, causing sudden, widespread hair loss (anagen effluvium). Nearly 65% of patients on chemotherapy experience complete scalp hair loss, according to the National Cancer Institute in 2019. Hair loss begins 1 to 3 weeks after starting treatment.
- Antidepressants (e.g., sertraline, fluoxetine, amitriptyline): Cause telogen effluvium by altering neurotransmitter levels that affect hair follicles. Hair loss occurs in 10–15% of patients using tricyclic antidepressants, according to a study published in “Dermatologic Clinics” (2013). SSRI-related hair loss is rare but reported in case studies.
- Blood pressure medications (beta-blockers, ACE inhibitors): The drugs slow follicle activity or push hair into the resting phase. Reported in less than 5% of users; more frequent in atenolol, metoprolol, and lisinopril users. Hair loss is listed as an uncommon side effect, according to FDA data.
- Anticoagulants (warfarin, heparin): Interfere with blood flow and follicle nutrient supply, leading to diffuse shedding. Telogen effluvium in some long-term heparin users, according to a journal of “Clinical and Aesthetic Dermatology review” (2015). Risk increases with prolonged use or high doses.
- Oral contraceptives and hormone therapies: Hormonal changes from birth control pills or hormone replacement therapy trigger shedding when starting or stopping. Especially common in women with androgen sensitivity or PCOS. Telogen effluvium is temporary and reversible.
- Retinoids (isotretinoin for acne): Disrupt the hair cycle and reduce sebaceous gland activity. Hair loss occurs in up to 10% of long-term users (American Academy of Dermatology).
- Antithyroid medications (methimazole, propylthiouracil): Cause telogen effluvium by disrupting thyroid hormone levels, which are critical for follicle growth. Hair loss due to medication is mistaken for symptoms of the thyroid disease itself.
- Antiepileptics (valproic acid, carbamazepine): Cause biotin deficiency or alter mineral absorption, leading to diffuse thinning. Studies show hair loss in up to 12% of valproate users, according to \ “Epilepsy & Behavior”, 2004.
What Illnesses Can Cause Hair Loss in Females?
The illnesses that can cause hair loss in females are listed below.
- Thyroid disorders (Hypothyroidism and Hyperthyroidism): Thyroid hormones regulate hair growth. Imbalances cause follicles to enter the resting phase early. Underactive and overactive thyroid leads to diffuse thinning. Patients with thyroid issues experienced hair loss, according to the study titled “Impact of Thyroid Dysfunction on Hair Disorders” by Ramadan S Hussein, dated 2023.
- Polycystic Ovary Syndrome (PCOS): PCOS causes elevated androgen levels, which shrink hair follicles and result in pattern thinning. Women with PCOS experience scalp hair loss and excess facial/body hair. Over 20% of women with PCOS report hair thinning, according to “The Journal of Clinical Endocrinology & Metabolism” dated 2010.
- Lupus (Systemic Lupus Erythematosus): Lupus is an autoimmune disease that inflames and damages hair follicles. It leads to patchy hair loss or scarring alopecia on the scalp. 45% of lupus patients had visible hair loss, according to “Lupus Science & Medicine” (2015).
- Iron deficiency anemia: Iron supports hair follicle metabolism. Low iron reduces oxygen delivery, leading to shedding. It is common in menstruating and pregnant women. Iron deficiency to telogen effluvium is over 60% of affected women, according to a study in “Dermatology Online Journal” (2006).
- Diabetes (Type 1 and 2): Poor circulation and high blood sugar levels damage follicles and impair growth. Diabetes causes stress-induced telogen effluvium or is linked to autoimmune alopecia areata. Higher rates of hair loss in diabetic females compared to non-diabetics, according to “Journal of Dermatology” (2013).
- Autoimmune disorders (alopecia areata, Hashimoto’s thyroiditis, psoriasis): The immune system attacks the body’s hair follicles. Disorders cause patchy, sudden loss or chronic scalp inflammation. Alopecia areata affects 2% of the population, with women more commonly affected, according to the “American Academy of Dermatology” (2010).
- Scalp infections (tinea capitis): Fungal infections inflame and destroy hair shafts, leading to scaly bald patches. Scalp infections are more common in children but are seen in adult women. Diagnosis is confirmed by culture or microscopy.
- Severe chronic illness or surgery: Major illnesses or surgical stress shock hair follicles into the resting phase. Hair loss appears 2 to 3 months after the event (telogen effluvium). Cleveland Clinic identifies it as a common post-hospitalization symptom.
Which Hormones Cause Hair loss in Females?
The hormones that cause hair loss in females are androgens, dihydrotestosterone (DHT), and imbalances in estrogen, progesterone, thyroid hormones, and prolactin. DHT is the primary hormone responsible for female pattern hair loss. It binds to androgen receptors in scalp follicles, causes follicle shrinkage, and shortens the hair growth cycle. DHT leads to thinner and weaker hair, especially in women with high androgen levels or increased sensitivity, such as individuals with polycystic ovary syndrome (PCOS). Estrogen supports hair growth by prolonging the anagen phase of the hair cycle. Hair enters the shedding phase when estrogen levels drop after childbirth or during menopause. Progesterone functions as a natural blocker of DHT. Androgens act more strongly on hair follicles when progesterone levels decrease, which is common in perimenopause.
Thyroid hormones (T3 and T4) are essential for normal follicle function. Hypothyroidism and hyperthyroidism disrupt the hair cycle and lead to telogen effluvium, which is a form of diffuse hair shedding. High levels of prolactin (hyperprolactinemia) interfere with the balance of estrogen and androgens and contribute to hair loss. The hormonal changes affect the hair growth cycle in different ways, according to the study titled ‘Hormonal Effects on Hair Follicles” by Monika Grymowicz, dated 2020.
How Does Hair Loss in Women Lead to Excessive Hair Fall and Shedding?
Hair loss in women leads to excessive hair fall and shedding by disrupting the normal hair growth cycle when more hair follicles shift into the telogen (resting) phase prematurely. 85–90% of scalp hair remains in the anagen (growth) phase, while only 10–15% is in the telogen phase. A larger number of hairs enter the resting phase and eventually shed when the balance is disturbed due to hair loss triggers, such as hormonal changes, stress, or illness.
Factors that cause excessive shedding include hormonal imbalances (menopause or thyroid dysfunction), nutritional deficiencies (low iron or vitamin D), stress-related telogen effluvium, and autoimmune diseases (alopecia areata). Each of the conditions affects the hair follicle’s ability to remain in the growth phase, resulting in increased daily shedding or sudden clumps of hair falling out. Women experiencing telogen effluvium had higher hair shedding rates compared to women with normal hair cycles, according to a study published in the International Journal of Trichology (2011). The study confirmed that stress, anemia, and endocrine disorders were leading contributors to the excessive shedding.
What Are the Treatments for Hair Loss in Women?
The treatments for hair loss in women are listed below.
- Minoxidil (Topical treatment): FDA-approved for female pattern hair loss. Expands blood vessels around follicles and prolongs the anagen (growth) phase. Applied as 2% or 5% solution once or twice daily. 5% minoxidil increased hair count and thickness after 24 weeks, according to a study in “Journal of the American Academy of Dermatology” (2014). It takes about 3 to 6 months to see noticeable improvement and is needed for women with early-stage thinning or diffuse shedding.
- Oral medications: Spironolactone blocks androgen receptors and lowers DHT, which causes follicle shrinkage. Finasteride is less commonly prescribed for women, but it is used off-label in postmenopausal cases. Results appear after 6 to 12 months of continuous use. Useful for women with high androgen levels, like PCOS. Spironolactone’s role in reducing female pattern hair loss progression, according to research in “Dermatologic Therapy” (2017).
- Low-Level Laser Therapy (LLLT): Uses red light to stimulate follicle activity and cell metabolism. Increases blood flow and reduces inflammation around follicles. Significant regrowth after 26 weeks using LLLT devices, according to a clinical trial in ‘Lasers in Surgery and Medicine’ dated 2014. Recommended for mild to moderate thinning and in combination with other treatments. Visible results take 4 to 6 months.
- Platelet-Rich Plasma (PRP) therapy: Involves injecting concentrated platelets from the patient’s blood into the scalp. Platelets release growth factors that repair damaged follicles and boost regrowth. Improvement in density and thickness after 3–4 sessions. Performed monthly, results appear within 3 to 6 months. It is used when minoxidil or oral options are not effective.
- Hair transplant surgery: Involves removing hair follicles from a dense area and transplanting them to thinning regions. Effective for permanent female pattern baldness that has not responded to medication. Requires 6 to 12 months for full results and is best for women with stable hair loss. Success rates exceed 90% in appropriately selected candidates, according to the “International Society of Hair Restoration Surgery (ISHRS)”.
- Hormonal therapy: Used to stabilize estrogen and progesterone levels in women with hormone-related shedding. It helps control hair loss in cases linked to menopause, PCOS, or hormonal imbalances. It takes 3 to 6 months to slow shedding. Most effective in premenopausal women with irregular cycles or confirmed hormonal shifts.
- Nutritional supplementation: Iron, zinc, vitamin D, biotin, and protein are critical for healthy hair growth. Supplements address underlying deficiencies that trigger telogen effluvium. Correcting iron and vitamin D deficiencies led to significant hair regrowth. It is needed for women with dietary gaps, anemia, or post-surgical recovery. Improvement appears within 2 to 4 months after correcting deficiencies.
- Corticosteroid injections or creams: Used for autoimmune hair loss like alopecia areata. Creams reduce local inflammation and prevent immune attack on follicles. Injections are given every 4–6 weeks; regrowth begins after 1–3 sessions. It is recommended for patchy bald spots or the sudden onset of shedding. Regrowth rates of 25–80% depending on severity, according to studies in “Archives of Dermatology” dated 2011 report. The options are considered part of Hair Loss Treatments that target inflammation-driven conditions and support localized follicle recovery.
How Effective Is Hair Transplant as a Solution for Hair Loss in Women?
Hair transplant is an effective solution for permanent hair loss in women, in cases where medical treatments have failed to restore hair volume. Hair transplantation is used to treat female pattern baldness, which involves thinning at the crown or along the part line. It becomes a viable option after medication-related hair loss has stabilized, ensuring that the underlying condition is no longer causing active shedding.
The procedure involves harvesting healthy hair follicles from a donor area, the back or sides of the scalp, and transplanting them to thinning or balding areas. FUE (Follicular Unit Extraction) and FUT (Follicular Unit Transplantation)are the two methods used. The follicles are genetically resistant to DHT, meaning they continue to grow even in areas affected by hair loss. The transplanted hair begins growing naturally within 3 to 4 months, with full results visible after 9 to 12 months. Success rates for hair transplants in properly selected female candidates exceed 90%. Women with stable, localized thinning and healthy donor density achieve natural-looking and permanent results.
Turkey has become a global hub for hair restoration, offering advanced procedures at competitive prices. The advantages of getting a hair transplant in Turkey are access to experienced surgeons, modern facilities, and all-inclusive packages that cover travel and post-op care. Vera Clinic is widely recognized as the best hair transplant clinic in Turkey, known for its medical excellence, FDA-approved techniques, and high patient satisfaction ratings.
What to Expect Before and After a Female Hair Transplant
Before and after a female hair transplant, patients follow a clear process involving preparation, surgery, recovery, and gradual regrowth. The doctor performs a detailed consultation to evaluate hair loss patterns, donor hair availability, and overall scalp health before the procedure. Medical reviews and blood tests help rule out active shedding conditions (telogen effluvium or thyroid disorders). Patients must stop smoking, avoid alcohol, and discontinue certain medications like blood thinners at least one week before surgery. It is common for women to have the donor area of their scalp trimmed. Full shaving is not required with the Follicular Unit Extraction (FUE) method.
Healthy follicles are extracted from the donor site and implanted into thinning or bald areas under local anesthesia during the procedure. The process takes between four and eight hours, depending on how many grafts are needed. Hospital admission is not necessary. Patients experience mild swelling, redness, and scabbing for about one week after surgery. It is important to avoid direct sun exposure, aggressive scalp washing, and the use of styling products for at least two weeks.
Hair in the transplanted area sheds within two to four weeks, a normal process known as shock loss. New hair starts growing around the third month. Visible improvement appears by six months, and full results are seen between nine and twelve months. Most women return to light activity after two to three days and resume work within a week. Final hair density depends on the quality of donor hair and how well the patient follows post-operative care instructions. A female hair transplant, when performed under stable hair loss conditions, offers a lasting solution to permanent thinning. The Hair Transplant Before and After expectations must be managed realistically, as results vary depending on hair type, donor supply, and individual recovery response.
When to See a Dermatologist for Hair Loss in Female
See a dermatologist for hair loss in females when the shedding becomes excessive, sudden, patchy, or continues for more than three months without improvement. Specific symptoms indicate the need for medical evaluation. Rapid thinning, a widening part, visible scalp, or sudden bald patches, which point to conditions like alopecia areata or scarring alopecia. Itching, burning, scaling, or pain in the scalp are other warning signs that suggest infection or inflammation. The signal telogen effluvium or an underlying illness such as iron deficiency, thyroid dysfunction, or an autoimmune disorder, if hairs fall increases to more than 150 strands a day or comes out in clumps when brushing or washing. Early diagnosis by a dermatologist improves the chance of reversing or controlling hair loss before it becomes permanent. A Hair Transplant Consultation is necessary in cases of advanced thinning or scarring where medical treatment has failed to restore density.
Are There Any Home Remedies to Stop Hair Loss in Women?
Yes, there are home remedies to stop hair loss in women, but it varies depending on the levels of scientific studies for its effectiveness. Scalp massage shows promise for increasing hair thickness, according to the study titled “Standardized Scalp Massage Results in Increased
Hair Thickness by Inducing Stretching Forces to Dermal Papilla Cells in the Subcutaneous Tissue” by Taro Koyama, dated 2016. Viviscal boosts hair strands, volume, coverage, and thickness. Fish oil, rich in omega-3s, promotes growth by extending the growth phase, though more research is needed. Ginseng stimulates growth and delays the end phase. Onion juice improves growth, with notable regrowth in alopecia areata cases. Rosemary oil is as effective as minoxidil, stimulating scalp blood flow. Geranium oil promotes growth in studies. Pumpkin seed oil increases regrowth. Saw palmetto reduces fallout and improves density. Green tea extracts increase density and diameter. Diets high in protein, iron, and fatty acids combat deficiencies involved in hair loss. The types of home remedies include nutritional adjustments, oral supplements, and topical application. Other types are coconut oil, rosemary oil, peppermint oil, red ginseng, and onion juice, according to the article titled “6 natural remedies to help with hair loss: Everything you need to know” by Katie Kindelan, dated 2023.
How to Prevent Extreme Hair Fall in Women
To prevent extreme hair fall in women, follow the nine steps below.
- Maintain a healthy diet. Eat iron-rich foods (spinach, lentils), proteins (eggs, fish), and vitamins (A, D, E, B12). Deficiencies are a major cause of extreme hair fall.
- Limit heat and chemical exposure. Avoid frequent use of straighteners, curlers, dyes, and bleach. These weaken the hair shaft and trigger breakage and shedding.
- Manage stress effectively. Practice regular sleep, meditation, or light exercise. Stress is linked to telogen effluvium, a common cause of extreme hair fall.
- Use gentle hair care products. Choose sulfate-free shampoos and moisturizing conditioners. Avoid products with harsh alcohols or artificial fragrances.
- Avoid tight hairstyles. Styles that pull the hair (ponytails or braids) cause traction alopecia. Allow the scalp to rest by alternating hairstyles.
- Check for hormonal or medical issues. Have the thyroid, iron, and vitamin D levels tested. Conditions like PCOS and hypothyroidism cause excessive shedding.
- Massage the scalp regularly. Boost blood flow to hair follicles by gently massaging with oils like coconut or rosemary. Improves follicle activity over time.
- Use clinically recommended treatments if needed. Apply minoxidil or take supplements under medical guidance. They support regrowth and reduce active loss.
- Stay hydrated. Drink enough water daily to keep hair and scalp healthy. Dehydration affects hair structure and worsens extreme hair fall.
How to Control Hair Fall for Women
To control hair fall in women, there are six steps. First, identify and treat any underlying health issues such as thyroid disorders, iron deficiency, or hormonal imbalances. Second, maintain a balanced diet rich in protein, iron, zinc, and essential vitamins like D and B12 to support healthy hair growth. Third, avoid excessive heat styling, harsh chemical treatments, and tight hairstyles that can damage the hair and strain the scalp. Fourth, use gentle, sulfate-free shampoos and conditioners that preserve natural oils and promote scalp health. Fifth, manage stress through regular exercise, meditation, or consistent sleep routines, as stress is a common cause of temporary hair shedding. Lastly, consider applying treatments like minoxidil or natural oils such as rosemary or coconut oil to stimulate hair follicles.
What Are the Common Types of Hair Loss in Women?
The common types of hair loss in women are listed below.
- Androgenetic Alopecia (Female Pattern Hair Loss): A genetic disorder associated with hormonal sensitivity to DHT. Leads to gradual thinning at the crown and widening of the part line.
- Telogen Effluvium in Women: Triggered by stress, illness, surgery, or nutritional deficiencies. A sudden, diffuse shedding of hair occurs as more follicles enter the resting phase.
- Traction Alopecia in Women: Result of repeated tension from tight hairstyles (braids, ponytails). Results in thinning or bald patches near the hairline and temples.
- Alopecia Areata in Women: An autoimmune condition where the immune system attacks hair follicles. Leads to sudden, patchy bald spots that regrow or spread.
- Anagen Effluvium in Women: Rapid hair loss during the growth phase, commonly due to chemotherapy or toxins. Hair falls out suddenly and involves the entire scalp.
- Cicatricial (Scarring) Alopecia in Women: An inflammatory skin disease that destroys hair follicles permanently. It leaves smooth, shiny bald patches and causes pain or itching.
- Trichotillomania in Women: A psychological condition involving compulsive hair-pulling. Leads to uneven hair loss, broken hairs, and visible damage.
1. Androgenetic Alopecia (Female Pattern Hair Loss)
Androgenetic Alopecia (Female Pattern Hair Loss) is the most common type of hair loss in women, affecting up to 50% of women by age 50, according to the Journal of the American Academy of Dermatology. Androgenetic Alopecia is caused by a genetic predisposition and increased sensitivity of hair follicles to androgens, dihydrotestosterone (DHT), even when androgen levels are normal. The condition begins in a woman’s 20s or 30s and progresses with age after menopause, when estrogen levels decline. Female AGA differs from the male version in appearance and progression, and it does not lead to complete baldness, the frontal hairline remains intact, and the thinning is concentrated along the crown and part line. The Ludwig Scale is used to classify the severity of thinning in women, ranging from slight widening of the part (Type I) to diffuse scalp thinning with visible scalp (Type III).
Androgenetic alopecia is non-scarring and irreversible, unlike other types of hair loss, though it is managed with treatment. Telogen effluvium is a temporary form of diffuse shedding triggered by stress, illness, or hormonal shifts and resolves on its own. Alopecia areata is autoimmune, leading to sudden round bald patches that regrow. Traction alopecia results from tight hairstyles and causes gradual thinning along the hairline or temples. It is reversible if caught early, but becomes permanent if scarring occurs. Cicatricial alopecia involves inflammation that destroys hair follicles and leads to permanent scarring, while trichotillomania is a behavioral disorder marked by repetitive hair pulling, producing patchy loss with broken hairs.
Female pattern hair loss is not always related to high hormone levels, but to how hair follicles respond to patients’ hormones. Studies link the condition to specific androgen receptor (AR) gene polymorphisms and family history. Treatment options such as topical minoxidil (2% or 5%) have been shown to improve hair density in about 60% of women. Oral medications like spironolactone and hormonal therapies slow progression in women with underlying hormonal sensitivity. Women suffer from androgenetic alopecia, a chronic, progressive condition that affects their hair worldwide.
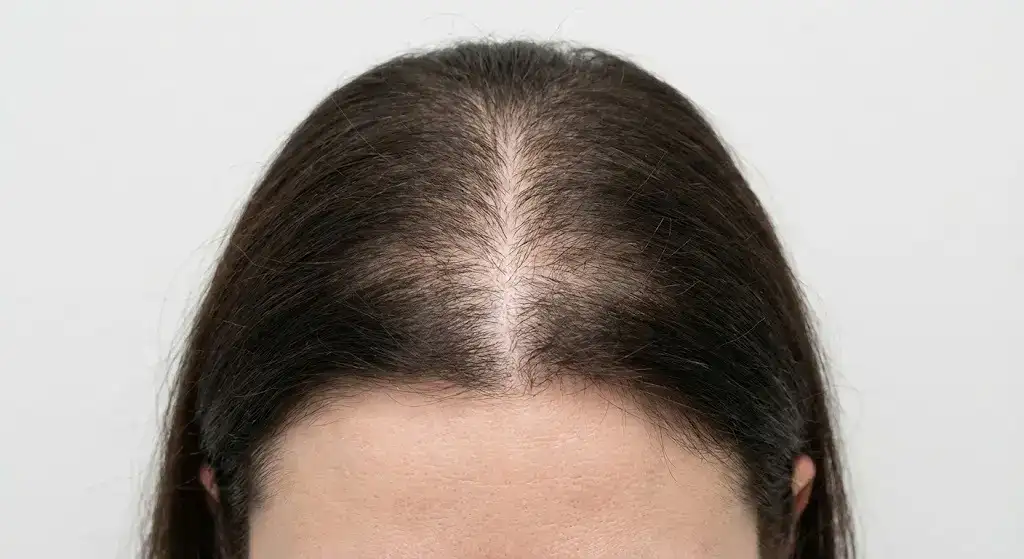
2. Telogen Effluvium in Women
Telogen Effluvium in Women is one of the most common causes of diffuse hair shedding in women, second only to androgenetic alopecia. Telogen Effluvium in Women occurs when a larger-than-normal number of hair follicles shift from the anagen phase into the telogen phase, leading to excessive shedding two to three months after a triggering event. The condition is prevalent in women due to hormonal fluctuations from childbirth, discontinuation of birth control, menopause, thyroid dysfunction, crash dieting, iron deficiency, and chronic stress, factors that more commonly affect women than men. The condition is acute and self-limiting, resolving within 6 months once the trigger is removed, though chronic telogen effluvium lasting longer than 6 months is possible to occur.
Telogen effluvium is unique to women because of their exposure to reproductive hormone shifts, including postpartum estrogen drop, perimenopause, and polycystic ovary syndrome (PCOS). It shows a stronger connection to dietary patterns and micronutrient deficiencies that are statistically more prevalent in women. Hair loss is diffuse across the scalp without a specific pattern, and the frontal hairline is preserved. The scalp appears normal without inflammation or scarring, and regrowth is possible once the trigger is addressed.
Androgenetic alopecia presents as gradual thinning of the crown and part line due to genetic and hormonal sensitivity, not linked to sudden stress. Alopecia areata is autoimmune, leading to sudden round bald patches with possible nail changes. Traction alopecia results from prolonged tight hairstyles and causes recession at the hairline or temples. Cicatricial alopecia is marked by inflammation and follicle destruction, resulting in permanent scarring and patchy bald areas. Trichotillomania, a psychological condition, causes irregular patches from repetitive pulling, with broken hairs at different lengths.
Telogen effluvium affects up to 30 to 50% of women at some point in their lives (American Family Physician, 2014). A 2018 study in the International Journal of Trichology confirmed higher rates among postpartum women and patients with iron deficiency. The hormonal and lifestyle triggers make it a far more frequent issue among women, while men experience telogen effluvium. Treatments focus on identifying and correcting the underlying cause, whether stress, nutritional deficiency, or hormone imbalance, after which normal growth resumes.
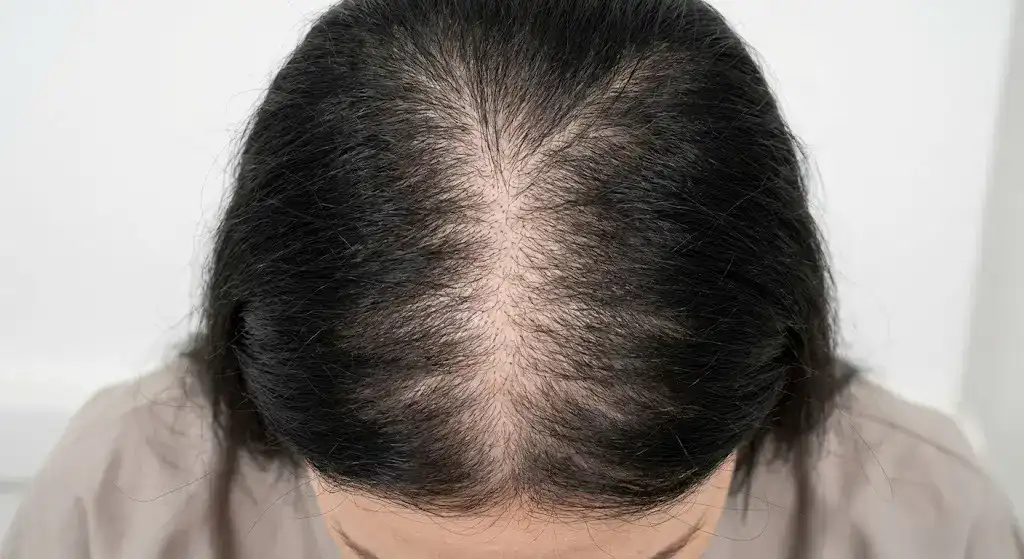
3. Traction Alopecia in Women
Traction Alopecia in Women is a common type of preventable hair loss. Traction Alopecia is caused by repeated tension or pulling on the hair. The condition is prevalent among women because of certain hairstyling practices. It includes tight ponytails, braids, weaves, extensions, buns, or head coverings that apply constant force on the hair follicles. The tension weakens the follicles and causes gradual hair loss. The loss starts around the front hairline and temples.
Traction alopecia is unique in women due to social and cultural styling practices. Men do not engage in the grooming methods. The condition is linked to beauty standards and the long-term use of chemical relaxers, tight cornrows, and heavy extensions. Hair loss in traction alopecia is localized. It starts at the edges and hairline. Broken hairs, a receding hairline, bumps, and redness are other signs of traction alopecia. Traction alopecia is non-scarring and reversible. It results in permanent follicle damage and scarring if the tension continues.
Androgenetic alopecia is hereditary. It causes progressive thinning at the crown and part line. Telogen effluvium leads to diffuse shedding after physical or emotional stress or hormonal shifts. Alopecia areata is an autoimmune condition. It causes sudden, round bald patches. Cicatricial alopecia involves inflammation that destroys follicles. It leads to permanent hair loss with scarring. Trichotillomania is a behavioral condition. It causes patchy hair loss due to repeated hair pulling and results in broken strands.
Traction alopecia affects up to 31.7% of African American women, according to research from the Journal of the American Academy of Dermatology in 2011. It makes it one of the most frequent types of hair loss in specific groups. Up to 50% of women who wear tight hairstyles for a long time show signs of follicle damage. Prevention and early intervention are essential. Changing hairstyles, reducing tension, and avoiding repeated trauma stop progression. Early-stage traction alopecia is fully reversible.
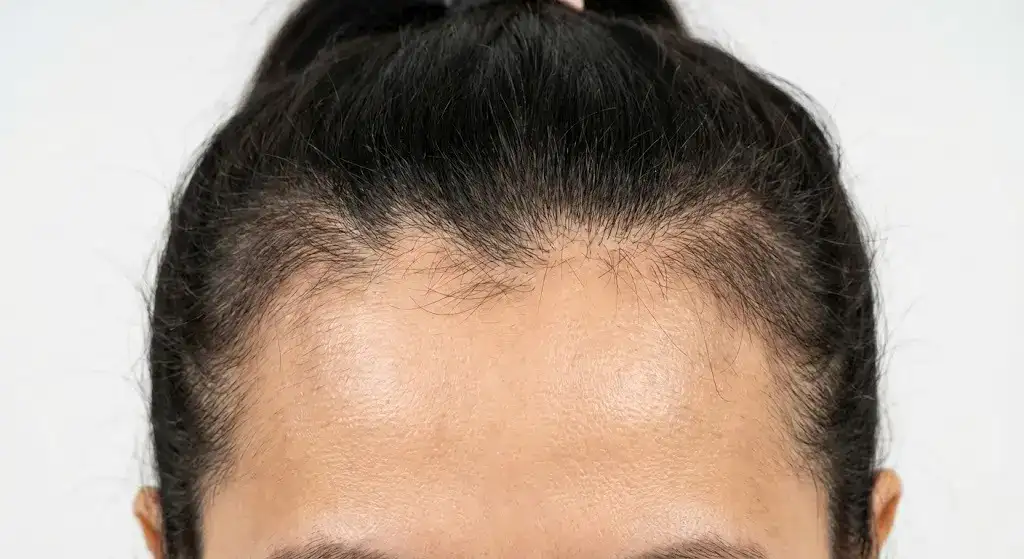
4. Alopecia Areata in Women
Alopecia Areata in Women is one of the most recognized autoimmune-related types of hair loss. Alopecia Areata occurs when the body’s immune system mistakenly attacks hair follicles, causing sudden and patchy hair loss. It is among the most common autoimmune-related hair loss conditions in women, while it is not the most common form overall. Its visibility, emotional impact, and unpredictable course make it a significant clinical concern. Women are more prone than men to experience autoimmune disorders, which increases their risk of developing alopecia areata.
Alopecia areata is unique in women due to its frequent connection with hormonal shifts, thyroid disease, and autoimmune conditions like lupus or Hashimoto’s thyroiditis. The condition worsens during periods of hormonal imbalance, such as pregnancy, menopause, or chronic stress. Hair loss in women presents as well-defined, round or oval bald patches that appear suddenly, on the scalp, eyebrows, or eyelashes. Women experience nail pitting or brittleness. The condition does not cause scarring, and hair regrowth is possible, unlike other types, although it falls out again.
Androgenetic alopecia causes gradual thinning along the crown and part line due to genetics and hormonal sensitivity. Telogen effluvium leads to diffuse shedding across the scalp, triggered by stress, illness, or hormonal changes. Traction alopecia results from tight hairstyles and affects the hairline or temples. Cicatricial alopecia causes scarring and permanent loss through inflammation and destruction of follicles. Trichotillomania is a behavioral disorder that causes patchy hair loss due to repeated hair pulling. 2.1% of the U.S. population develops alopecia areata in their lifetime, with women being slightly more affected than men, according to the National Alopecia Areata Foundation. Women made up over 60% of alopecia areata cases seen in dermatology clinics. Alopecia areata starts before age 40 and is linked with a family history of autoimmune disease. Treatment includes corticosteroid injections, topical immunotherapy, and JAK inhibitors, though response varies. Early diagnosis and autoimmune screening are recommended for women who present with sudden patchy hair loss.
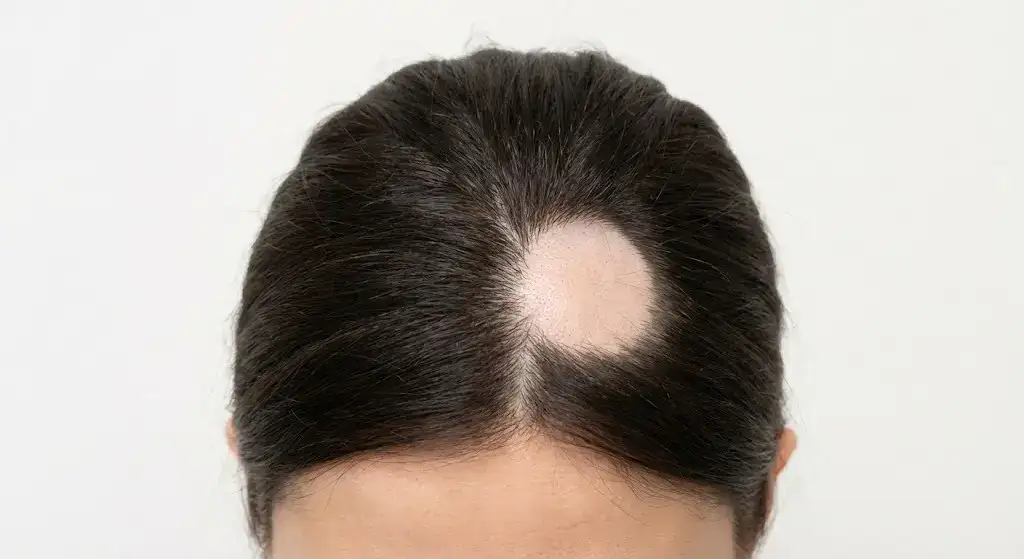
5. Anagen Effluvium in Women
Anagen Effluvium in Women is a sudden and severe type of hair loss that happens during the anagen or growth phase of the hair cycle. Anagen Effluvium in Women is most seen in women who are undergoing chemotherapy or radiation therapy as part of cancer treatment. It is one of the most frequent causes of rapid and widespread hair loss in women receiving medical treatments, while it is not the most common type of hair loss overall. Women are more prone than men to receive treatments for breast, ovarian, or uterine cancers. It makes them more affected by anagen effluvium.
Anagen effluvium is unique in women because many cancer types treated with chemotherapy primarily affect females. Chemotherapy drugs used for breast cancer, such as anthracyclines and taxanes, attack fast-dividing cells in the hair matrix. It causes hair to fall out within days or weeks after starting treatment. Hair loss is diffuse and affects the scalp, eyebrows, eyelashes, and body hair. The scalp becomes tender. The hair breaks off at the scalp surface, unlike other hair loss types. Regrowth begins one to three months after treatment ends. The new hair grows back with a different texture or color.
Androgenetic alopecia causes slow thinning at the crown and part line due to genetics and hormone sensitivity. Telogen effluvium results in diffuse shedding weeks after a stressor such as illness, childbirth, or surgery. Alopecia areata leads to sudden, round bald patches from an autoimmune reaction. Tight hairstyles cause traction alopecia and show hair loss near the hairline or temples. Cicatricial alopecia involves inflammation that destroys follicles and leads to permanent hair loss with scarring. Trichotillomania causes patchy hair loss due to compulsive hair pulling and results in broken strands.
Anagen effluvium affects up to 65 percent of women who receive standard chemotherapy for breast cancer, according to the Journal of Clinical Oncology. 75% of female patients considered hair loss the most distressing side effect of chemotherapy. It has a strong emotional impact, although hair loss from anagen effluvium is temporary. Scalp cooling devices, cold caps, and newer drug protocols are used to reduce the risk. Early education and psychological support help women manage the effects of the Anagen effluvium.
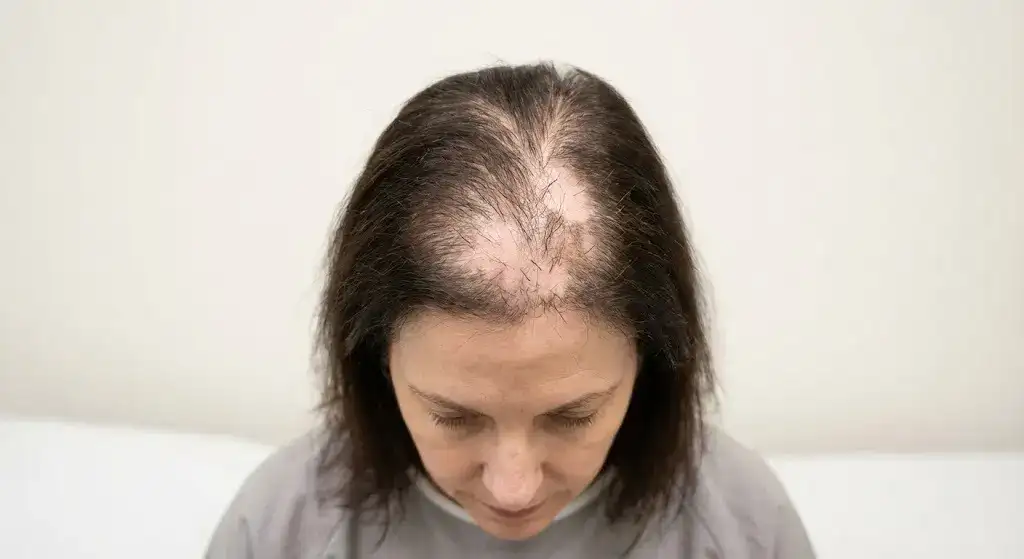
6. Cicatricial (Scarring) Alopecia in Women
Cicatricial (Scarring) Alopecia in Women is a less common but serious type of permanent hair loss. Cicatricial occurs when inflammation destroys hair follicles and replaces them with scar tissue. It is the most common type of irreversible hair loss in women, while it is not the most common form overall. The condition leads to permanent damage that unable to be reversed, making early detection critical. Cicatricial alopecia includes multiple disorders, such as lichen planopilaris, frontal fibrosing alopecia, and central centrifugal cicatricial alopecia (CCCA), many of which predominantly affect women.
Cicatricial alopecia is unique in women due to certain subtypes that primarily or exclusively affect them. Frontal fibrosing alopecia affects postmenopausal women and causes recession along the front hairline and eyebrows. Central centrifugal cicatricial alopecia is most common in women of African descent and starts at the crown, progressing outward. The forms are linked to hair care practices, hormonal changes, and autoimmune responses that disproportionately affect women. The affected areas show scalp redness, burning, scaling, or pustules. Follicles are destroyed and replaced by scar tissue, preventing regrowth.
Androgenetic alopecia causes slow thinning along the part line and crown due to hormonal and genetic factors. Telogen effluvium results in diffuse shedding from physical or emotional stress. Alopecia areata leads to patchy bald spots from autoimmune attacks. Traction alopecia results from repeated tension from hairstyles and affects the temples or hairline. Anagen effluvium causes sudden widespread hair loss during chemotherapy. Trichotillomania creates patchy hair loss with broken strands due to repeated pulling.
Cicatricial alopecia affects up to 3 to 7 percent of patients with hair loss, but it is underdiagnosed in women, according to research in the International Journal of Trichology. 80 % of frontal fibrosing alopecia cases occurred in women, mostly over age 50. CCCA was present in up to 5.6 % of African American women. Treatments include anti-inflammatory drugs, corticosteroids, and immunosuppressants, but the drugs are effective before permanent scarring occurs. Early recognition and intervention are essential to stop disease progression in women with Cicatricial (Scarring) Alopecia.
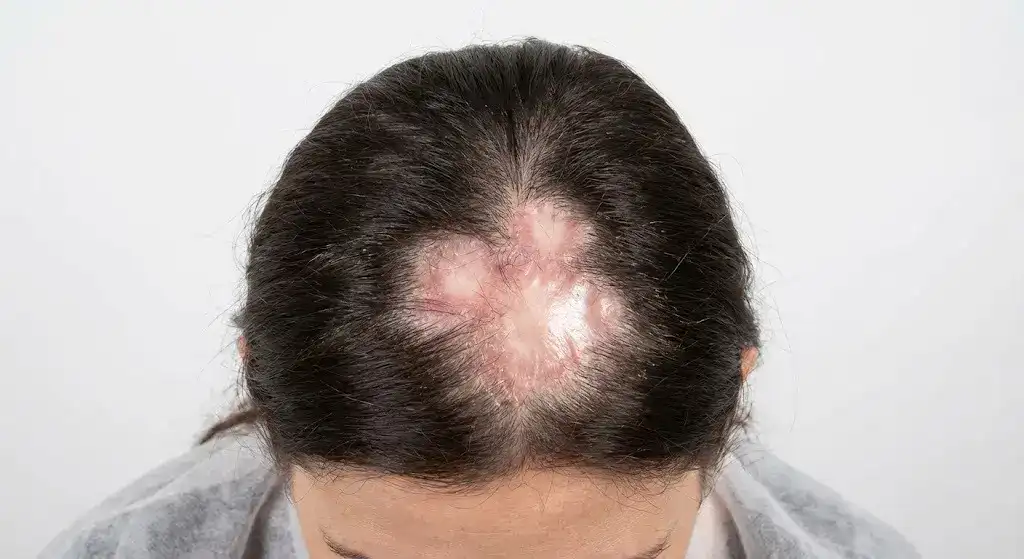
7. Trichotillomania in Women
Trichotillomania in Women is a psychological hair-pulling disorder that leads to patchy hair loss. Trichotillomania is one of the most common impulse control–related causes of hair loss in women, while it is not the most common cause of hair loss overall. The condition is classified under obsessive-compulsive and related disorders and involves recurrent, irresistible urges to pull out hair from the scalp, eyebrows, eyelashes, or other areas. Trichotillomania disproportionately affects women, with females representing 70 to 90 % of diagnosed cases, during adolescence and adulthood.
Trichotillomania is unique in women because it emerges during puberty, a time of hormonal and emotional changes that increase vulnerability to anxiety and compulsive behaviors. Many women report pulling in response to stress, boredom, or negative emotions. The condition is concealed for years due to shame or embarrassment, which delays diagnosis. Hair loss is irregular and patchy, with broken hairs of varying lengths. The hair loss pattern does not follow medical or hormonal causes, unlike other forms. Women exhibit trichophagia, or the habit of eating pulled hair, which leads to digestive complications.
Each hair loss condition in women has distinct clinical traits. Androgenetic alopecia presents as gradual thinning at the crown and part line due to hormone sensitivity. Telogen effluvium causes diffuse shedding after stress or illness. Alopecia areata results in sudden, round bald spots caused by autoimmune attacks. Traction alopecia is caused by tension from hairstyles and affects the hairline or temples. Cicatricial alopecia causes permanent loss due to inflammation and follicle destruction. Anagen effluvium causes rapid, widespread hair loss during chemotherapy.
Trichotillomania affects up to 2.5 percent of the population, with a higher rate in women, according to the American Journal of Psychiatry. 1 in 50 women are affected patients between the ages of 12 and 30. It is common for trichotillomania to coexist with depression, anxiety, or obsessive-compulsive traits. Cognitive behavioral therapy, habit reversal training, is the first-line treatment. Medications such as SSRIs or N-acetylcysteine have shown benefit in some cases. Early mental health support is essential to reduce hair damage and improve emotional well-being.
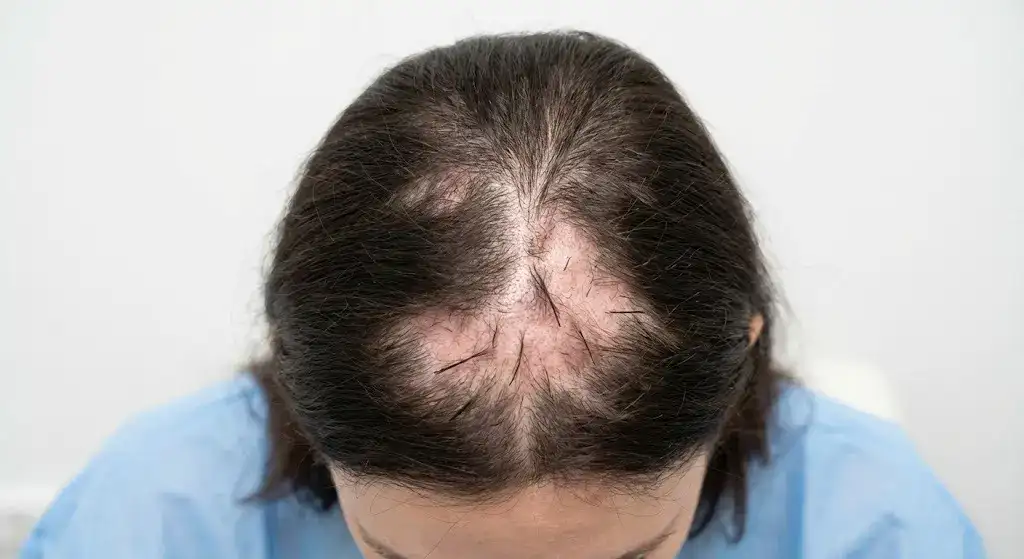
What Are the Rare Types of Hair Loss in Women?
The rare types of hair loss in women are listed below.
- Cicatricial (Scarring) Alopecia: A group of rare disorders where inflammation permanently destroys hair follicles and replaces them with scar tissue. Includes conditions like lichen planopilaris, frontal fibrosing alopecia (FFA), and discoid lupus erythematosus. Major characteristics: smooth, shiny bald patches, scalp pain, burning, or itching. Affects less than 3% of women with hair loss, according to the Journal of the American Academy of Dermatology (2018). Considered rare due to its irreversible nature and need for early biopsy confirmation.
- Anagen Effluvium: Sudden loss of actively growing hair, due to chemotherapy, radiation, or toxins. Major characteristics include rapid hair loss within days or weeks of exposure, affecting the entire scalp or body. Seen in approximately 65% of female chemotherapy patients, as per National Cancer Institute data. Rare in the general population and mainly treatment-induced.
- Trichotillomania: A compulsive hair-pulling disorder classified as a psychiatric condition. Major characteristics include uneven hair patches, broken hairs, and repeated pulling behavior, affecting the scalp, brows, or lashes. Affects about 1–2% of females, most commonly during adolescence (American Psychiatric Association, DSM-5). Considered rare because it is behavior-driven and misdiagnosed.
- Congenital Hypotrichosis and Genetic Hair Disorders: Inherited conditions causing sparse or absent hair from birth or early childhood. Major characteristics: abnormal hair texture, absent eyebrows or lashes, and associated with ectodermal dysplasia. Extremely rare, with prevalence rates <1 in 10,000 births, according to Orphanet Journal of Rare Diseases. Diagnosed through genetic testing and early clinical signs.
- Loose Anagen Syndrome: Hair easily pulls out during the anagen (growth) phase without pain or inflammation. Major characteristics: hair fails to grow long, appears thin, and falls out with minimal effort. Seen mainly in young girls aged 2–6 and rarely persists into adulthood. Considered rare due to its self-limiting nature and age specificity.
Rare types of hair loss in women are influenced by age, demographics, genetics, and underlying health conditions. Age-specific conditions include loose anagen syndrome in young girls and frontal fibrosing alopecia in postmenopausal women. Certain types, such as Central Centrifugal Cicatricial Alopecia (CCCA), are more common in specific ethnic groups due to styling practices. Genetic disorders like congenital hypotrichosis appear early in life and are inherited. Autoimmune diseases and psychological disorders trigger conditions like scarring alopecia, alopecia areata, and trichotillomania. Understanding the factors is essential for accurate diagnosis and effective treatment.