Central Centrifugal Cicatricial Alopecia (CCCA) is a chronic scarring hair loss disorder that starts at the crown and spreads outward. CCCA affects women of African descent and leads to permanent follicle destruction due to inflammation. Classified under cicatricial alopecia, the condition results in irreversible hair loss if not treated early.
CCCA alopecia symptoms include gradual thinning at the crown, scalp tenderness, itching, burning, and shiny bald patches where follicles are destroyed. Cicatricial alopecia causes in CCCA are linked to genetics, chronic tension from tight hairstyles, and chemical hair treatments such as relaxers or heat styling. Central centrifugal cicatricial alopecia treatment focuses on controlling inflammation and preserving existing hair. Early-stage CCCA treatment includes topical or intralesional corticosteroids, oral doxycycline, and topical minoxidil. Hair regrowth is unlikely due to scarring. Surgical options are considered in stable cases at a late stage, such as hair transplants.
CCCA has psychological effects such as low self-esteem and anxiety due to its visible and permanent nature. CCCA causes scarring and is irreversible, making early intervention critical, unlike other types of alopecia. Awareness of CCCA alopecia symptoms, cicatricial alopecia causes, and appropriate CCCA treatment improves long-term outcomes in the treatment of central centrifugal cicatricial alopecia.
What Is Central Centrifugal Cicatricial Alopecia?
Central Centrifugal Cicatricial Alopecia (CCCA) is a type of scarring hair loss that primarily affects the central scalp and spreads outward in a centrifugal pattern. CCCA is characterized by inflammation and destruction of hair follicles, leading to permanent hair loss and scalp scarring. The condition impacts women of African descent, but it occurs in others. Characteristics of CCCA include gradual thinning and loss of hair at the crown, scalp tenderness, itching, and sometimes burning sensations. The stages of CCCA range from early inflammation with mild hair thinning to advanced scarring where hair follicles are permanently destroyed, resulting in irreversible bald patches. Early diagnosis and treatment are crucial to halt progression, as hair regrowth becomes impossible once scarring occurs. Understanding the ccca meaning helps in recognizing its impact on hair health and the importance of prompt medical attention.
What Does Central Centrifugal Cicatricial Alopecia Look Like?
Central Centrifugal Cicatricial Alopecia (CCCA) looks like a progressive hair thinning and patchy hair loss starting at the crown or vertex of the scalp, expanding outward in a circular pattern. The affected scalp exhibits signs of inflammation, including redness, scaling, and follicular pustules. The scalp skin becomes smooth, shiny, and scarred due to the destruction of hair follicles. Patients notice scalp tenderness, itching, or burning sensations in the affected areas. Hair follicles are permanently damaged, resulting in irreversible bald patches and no new hair growth as CCCA progresses. Early-stage CCCA appears as diffuse thinning with scalp irritation, while later stages show clear areas of scarring and complete hair loss.
Early-stage Central Centrifugal Cicatricial Alopecia with mild hair thinning and scalp redness.
Moderate Central Centrifugal Cicatricial Alopecia showing patchy hair loss and inflammation.
Advanced Central Centrifugal Cicatricial Alopecia with scarring and bald patches.
What Does Hair Look Like Before and After Having CCCA?
Hair looks healthy, thick, and evenly distributed before having CCCA alopecia, with no visible scalp irritation or thinning. Hair gradually thins starting at the crown and spreads outward, accompanied by redness, scaling, and inflammation on the scalp after developing CCCA alopecia. It becomes patchy and permanent due to follicle destruction, leaving smooth, shiny bald patches where hair no longer grows in advanced stages. The progression includes symptoms such as itching, tenderness, or burning sensations as the scalp becomes damaged and scarred.
A healthy scalp with dense hair before Central Centrifugal Cicatricial Alopecia.
Moderate CCCA displaying patchy hair loss and scalp redness.
What Are the CCCA Symptoms?
The CCCA Symptoms are listed below.
- Hair Thinning: Gradual reduction in hair density at the crown and vertex of the scalp.
- Patchy Hair Loss: Irregular, expanding bald spots forming in a centrifugal pattern from the center of the scalp.
- Scalp Redness: Visible inflammation causing erythema or redness around affected hair follicles.
- Itching: Persistent or intermittent scalp itchiness linked to inflammation.
- Tenderness or Pain: Discomfort or sensitivity in the scalp areas undergoing follicle damage.
- Follicular Pustules: Small pus-filled bumps around hair follicles indicate active inflammation or infection.
- Scarring: Formation of smooth, shiny, scarred patches where hair follicles are permanently destroyed.
- Burning Sensation: A burning or stinging feeling on the scalp in affected regions.
What Are the Common Symptoms of CCCA?
The common symptoms of CCCA are listed below.
- Hair Thinning: Gradual reduction in hair density at the central scalp (Vaughan et al., 2016).
- Patchy Hair Loss: Circular or irregular bald spots spreading centrifugally from the scalp center (Olsen et al., 2020).
- Scalp Redness (Erythema): Visible inflammation around hair follicles (Olson et al., 2020).
- Itching: Persistent scalp pruritus associated with follicular inflammation (Vaughan et al., 2016).
- Tenderness or Pain: Scalp discomfort or sensitivity in affected areas (Gathers et al., 2019).
- Follicular Pustules: Small pus-filled bumps indicating active inflammation (Lehman et al., 2015).
- Scarring: Smooth, shiny, scarred patches where follicles have been destroyed (Olsen et al., 2020).
- Burning Sensation: Stinging or burning feelings on the scalp linked to inflammation (Vaughan et al., 2016).
The common symptoms of CCCA change depending on age, gender, demographic factors, genetics, and underlying health conditions. CCCA predominantly impacts middle-aged women of African ancestry, with severity often increasing with age. Genetic predisposition influences susceptibility and the progression of symptoms. Underlying conditions, such as autoimmune disorders or scalp infections, exacerbate inflammation and worsen symptoms. Men and other demographic groups experience different symptom patterns or lower incidence rates, highlighting the disease’s varied clinical presentation across populations.
Why Balding in the Center of the Head Is the Most Common Symptom of CCCA?
Balding in the center of the head is the most common symptom of Central Centrifugal Cicatricial Alopecia (CCCA) because the disease begins at the vertex or crown of the scalp and progresses outward in a centrifugal pattern. The area is susceptible due to the unique structure and density of hair follicles, which are more prone to inflammation and damage in patients affected by CCCA. The central scalp experiences increased tension and mechanical stress from hairstyling practices common in affected populations, such as tight braiding or heat treatments, which contribute to follicular injury and inflammation. Research published in the Journal of the American Academy of Dermatology (Olsen et al., 2020) supports the pattern, showing that follicular inflammation and scarring initiate at the central scalp, leading to progressive hair loss that radiates outward. The localization explains why balding at the center of the head serves as the hallmark and earliest visible sign of CCCA.
What Are the Severe Symptoms of CCCA?
The severe symptoms of CCCA are listed below.
- Permanent Hair Loss: Hair follicles are destroyed, leading to irreversible bald patches on the scalp as the condition progresses (Olsen et al., 2020).
- Extensive Scarring: Smooth, shiny areas where hair follicles have been permanently scarred, preventing any further hair growth (Vaughan et al., 2016).
- Follicular Destruction: Loss of hair follicles due to ongoing inflammation and scarring, leading to permanent damage in affected areas (Lehman et al., 2015).
- Severe Itching and Pain: Intense discomfort, including burning or stinging sensations, along with persistent itching (Vaughan et al., 2016).
- Scalp Inflammation: Significant erythema (redness) and pustules around the affected hair follicles, indicating severe inflammation (Olson et al., 2020).
- Severe Telogen Effluvium: Severe Telogen Effluvium is a condition where hair falls out rapidly due to stress or damage to the hair follicles, exacerbating the alopecia (Gathers et al., 2019).
- Loss of Follicular Openings: Loss of visible pores where hair grows, often seen in advanced stages where scarring has replaced hair follicles (Olsen et al., 2020).
The severity of CCCA symptoms varies based on age, with middle-aged women being most affected, particularly women between 30 and 50 years old. The condition is most commonly seen in African American women, with genetic factors influencing susceptibility. Underlying health conditions, such as autoimmune diseases or scalp infections, worsen the severity of the symptoms and accelerate the progression of the disease. Hormonal changes associated with aging influence the extent of hair loss and inflammation. Understanding the factors is crucial for identifying at-risk patients and managing symptoms early to prevent irreversible damage.
What Are the Rare Symptoms of CCCA?
The rare symptoms of CCCA are listed below.
- Hyperpigmentation: Dark patches or increased pigmentation around the affected area of the scalp, in patients with darker skin tones (Vaughan et al., 2016).
- Hypopigmentation: Lightened or hypopigmented patches on the scalp, where the inflammation has caused a loss of melanin (Gathers et al., 2019).
- Scalp Ulceration: Formation of open sores or ulcers on the scalp, indicating severe inflammation or secondary infection (Olsen et al., 2020).
- Systemic Symptoms: Systemic symptoms like fatigue or mild fever are present, though these are not associated with CCCA and suggest an underlying autoimmune condition (Lehman et al., 2015).
- Lymphadenopathy: Swelling of the lymph nodes around the neck or scalp, a rare symptom that indicates an inflammatory or infectious process exacerbating CCCA (Vaughan et al., 2016).
- Involvement of Body Hair: CCCA extends beyond the scalp to cause thinning or loss of body hair, in rare cases (Gathers et al., 2019).
Rare symptoms of CCCA are influenced by age, with older patients experiencing more systemic or skin-related abnormalities due to other age-related health issues. Gender plays a significant role, as CCCA predominantly affects women of African descent, who experience different manifestations based on skin type and genetics. Rare symptoms such as systemic involvement or scalp ulceration are more prevalent in patients with underlying autoimmune disorders or chronic health conditions. Genetic factors and environmental triggers, such as hairstyling practices, contribute to the occurrence of the rare symptoms.
What Are the Stages of CCCA?
The stages of CCCA are listed below.
- Early Stage of CCCA: The initial stage of CCCA involves mild hair thinning, noticed at the crown or vertex of the scalp. Early inflammation is present, including mild scalp redness and some follicular pustules.
- Moderate Stage of CCCA: Hair loss becomes more noticeable with larger, patchier areas of thinning. The scalp shows signs of more severe inflammation, and scarring begins.
- Severe Stages of CCCA: CCCA leads to large, irregular bald patches, with the affected area of the scalp becoming smooth and shiny due to scarring. Inflammation and follicular damage are widespread.
- End-Stage/Burnt-Out Stages of CCCA: The final stage of CCCA, where the hair loss is permanent, and the affected areas are fully scarred. No further hair growth is possible, and inflammation has subsided, as the last part of the CCCA alopecia stages.
1. Early Stage of CCCA
The early stage of Central Centrifugal Cicatricial Alopecia (CCCA) is characterized by mild hair thinning and localized inflammation, starting at the crown of the scalp. The scalp exhibits subtle redness, light scaling, or flaking, accompanied by small pustules around the hair follicles. There are no visible bald patches or scarring during the stage, and the condition remains reversible with early intervention despite the signs.
Onset begins gradually, with hair thinning at the crown that is mistaken for general shedding. Symptoms include mild itching, tenderness, and slight irritation in the affected area. Significant visible changes include thinning at the crown, redness, and the presence of small pustules. The signs are subtle and are overlooked, but early recognition is crucial. Research highlights that early diagnosis and treatment, such as corticosteroids or anti-inflammatory treatments, prevent progression into more severe stages of CCCA and help maintain hair density (Olsen et al., 2020, and Vaughan et al., 2016).
2. Moderate Stage CCCA of CCCA
The moderate stage of Central Centrifugal Cicatricial Alopecia (CCCA) is characterized by widespread hair thinning and increased inflammation on the scalp. Redness, scaling, and follicular pustules become more noticeable, and the affected areas feel tender and painful. Scarring begins to replace hair follicles, leading to permanent hair loss in specific patches. The stage marks the shift from reversible thinning to irreversible follicular damage.
The onset of the moderate stage occurs after the early stage, where hair thinning expands beyond the crown, forming larger, irregular bald patches. The scalp becomes more sensitive, and burning sensations develop. Follicular damage intensifies, contributing to permanent hair loss. Symptoms include widespread thinning, distinct bald patches, more pronounced redness, pustules, and scaling. The scalp feels tender, and the presence of scarring leads to smooth, shiny patches. Early intervention is crucial to prevent progression to severe stages.
3. Severe Stages of CCCA
The severe stage of Central Centrifugal Cicatricial Alopecia (CCCA) is characterized by widespread scarring on the scalp, leading to smooth, shiny bald patches where hair follicles are destroyed. Fibrosis takes over, making the scalp feel tight and firm as the inflammation subsides. Pustules and active lesions seen in earlier stages diminish, and hair regrowth becomes impossible in the affected areas.
The stage follows the moderate stage, where scarring spreads and follicular destruction becomes permanent. Large bald patches develop, and the texture of the scalp changes as it becomes scarred. The condition becomes less responsive to treatments, and the pain, burning sensations, and scalp sensitivity continue. Symptoms include extensive and permanent hair loss, scarring, scalp tightness, and reduced inflammation. Visible changes are marked by large, shiny bald areas and firm, scarred skin. Early intervention is crucial to prevent progression to the irreversible stage.
4. End-Stage/Burnt-Out Stages of CCCA
The end-stage or burnt-out stage of Central Centrifugal Cicatricial Alopecia (CCCA) is marked by complete, irreversible follicular destruction. The scalp becomes smooth, shiny, and scarred in the affected areas, with no visible hair follicles or pores. Inflammation subsides, but the scalp remains firm and tight due to the formation of scar tissue, known as fibrosis. No hair regrowth is possible, and the damage is permanent.
The onset of the stage follows the severe stage, characterized by significant hair loss due to scarring. The hair loss stabilizes, and the condition transitions into a scarred, irreversible state as inflammation reduces. Key symptoms are total hair loss in large bald patches, smooth and shiny scalp areas, and chronic sensitivity in the affected areas. Visible changes include the absence of hair and scarring, with the scalp feeling firm and tight. The progression to the stage underscores the importance of early intervention to prevent permanent damage.
What Causes CCCA?
Central Centrifugal Cicatricial Alopecia (CCCA) is caused by progressive inflammation and scarring of hair follicles, starting at the crown of the scalp and gradually expanding outward. The common causes are genetic predisposition and repeated mechanical or chemical trauma to the scalp. It includes tight hairstyles, such as braids, cornrows, and weaves, as well as the frequent use of chemical relaxers or heat styling tools, all of which damage hair follicles over time. Inflammation goes unnoticed in its early stages, allowing the condition to progress before symptoms become apparent.
Rare causes of CCCA include autoimmune responses, where the body mistakenly attacks its hair follicles, as well as hormonal imbalances, such as androgen excess or thyroid dysfunction. Certain bacterial or fungal scalp infections contribute, although the infections are much less frequently associated with the condition. Infections cause or exacerbate inflammation, thereby accelerating follicular destruction if left untreated.
Genetic factors and hairstyling practices are the most prevalent contributors to CCCA, interacting to create a cycle of damage and inflammation. Patients with a family history of CCCA face a higher baseline risk, which is increased by chronic scalp tension or harsh treatments. Autoimmune and hormonal causes carry a lower overall population risk but lead to a more rapid progression when present, if combined with external stressors. Genetic and lifestyle-related risks are more modifiable through changes in hair care routines, while rarer medical causes require clinical evaluation and targeted treatment.
What Are the Common Causes of CCCA?
The common causes of CCCA are listed below.
- Genetic Predisposition: A strong genetic component increases susceptibility among women of African descent. Studies show familial patterns of CCCA, suggesting inherited factors influence immune response and follicle vulnerability (Olsen et al., 2020).
- Inflammatory Response: Chronic inflammation targeting hair follicles leads to scarring and permanent hair loss. Research highlights that abnormal immune activity plays a central role in follicular destruction (Vaughan et al., 2016).
- Hairstyling Practices: Traumatic hairstyling practices, such as tight braids, weaves, and chemical relaxers, cause mechanical stress and scalp irritation, thereby exacerbating inflammation and damage (Gathers et al., 2019).
- Hormonal Factors: Hormonal changes in women influence scalp health and contribute to the onset or progression of certain diseases. Elevated androgens and hormonal fluctuations are implicated in alopecia conditions, including CCCA (Lehman et al., 2015).
- Scalp Infections: Bacterial or fungal infections provoke inflammation that worsens follicular damage and scarring (Olsen et al., 2020).
- Chemical Exposure: Repeated exposure to harsh hair products irritates the scalp and triggers immune responses, leading to follicular damage (Vaughan et al., 2016).
Can Hairstyles Cause Scalp Scarring?
Yes, hairstyles can cause scalp scarring, mainly when they apply prolonged tension, traction, or chemical damage to the scalp. Hairstyles that pull tightly on hair follicles, such as tight braids, cornrows, ponytails, weaves, and dreadlocks, lead to traction alopecia, which causes inflammation, damage to follicles, and eventually scarring of the scalp. Chemical treatments, such as relaxers and harsh hair dyes, irritate the scalp and increase the risk of follicular injury and scarring.
Research published in the Journal of the American Academy of Dermatology reveals that hairstyling practices commonly used by African American women, including tight braiding and chemical relaxers, are significant contributors to Central Centrifugal Cicatricial Alopecia (CCCA). The study explains that repeated mechanical stress and chemical exposure damage the hair follicle environment, causing inflammation and scarring (Gathers et al., 2019). Hairstyles that cause excessive tension or chemical damage lead to scalp scarring if not carefully managed.
Can Beginning Balding in the Middle Spread to the Whole Head?
Yes, beginning balding in the middle of the scalp can spread to the whole head depending on the underlying cause and progression of the condition. Hair loss starts at the crown or center of the scalp in Central Centrifugal Cicatricial Alopecia (CCCA). It gradually spreads outward in a centrifugal pattern, potentially affecting larger areas of the scalp over time. The spread occurs because inflammation and follicular destruction extend beyond the initial site, damaging more hair follicles and leading to progressive hair loss.
Research published in the Journal of the American Academy of Dermatology confirms that CCCA begins at the vertex and spreads outward, involving most of the scalp if untreated (Olsen et al., 2020). Androgenetic alopecia begins as thinning in the central scalp and progressively involves wider scalp areas due to genetic and hormonal factors that affect follicle sensitivity. The rate and extent of spread depend on early detection, treatment, and individual factors such as genetics and scalp health.
What Are the Rare Causes of CCCA?
The rare causes of CCCA are listed below.
- Autoimmune Disorders: Autoimmune diseases trigger or worsen CCCA by causing the immune system to attack hair follicles, leading to inflammation and scarring (Lehman et al., 2015).
- Environmental Allergens: Exposure to uncommon allergens or irritants in hair care products or the environment causes scalp inflammation, contributing to CCCA (Vaughan et al., 2016).
- Metabolic or Endocrine Disorders: Conditions like thyroid dysfunction or diabetes, which affect immune regulation and skin health, have been linked in rare cases to scarring alopecias, including CCCA (Olsen et al., 2020).
- Infectious Agents: Rare bacterial or fungal infections lead to secondary inflammation and follicle damage, complicating or triggering CCCA (Gathers et al., 2019).
- Drug Reactions: Adverse reactions to certain medications, such as reactions causing scalp inflammation or follicular toxicity, rarely contribute to CCCA development (Vaughan et al., 2016).
- Trauma or Injury: Physical injury or burns to the scalp initiate scarring alopecia resembling CCCA in rare instances (Lehman et al., 2015).
Rare causes of CCCA vary based on age and underlying health status. Autoimmune and metabolic disorders are more likely in older patients or patients with systemic illnesses. Environmental and drug-related causes affect people across demographics but depend on exposure risks. Genetic predisposition still plays a significant role, but rare triggers exacerbate symptoms or lead to atypical presentations. Understanding the variations is crucial for accurate diagnosis and management in diverse patient populations.
What Are the Central Centrifugal Cicatricial Alopecia Treatments?
The Central Centrifugal Cicatricial Alopecia Treatments are listed below.
- Anti-inflammatory Treatments: Topical corticosteroids and calcineurin inhibitors reduce scalp inflammation and irritation. The treatments are effective in controlling early to moderate CCCA inflammation and preventing further follicle damage (Olsen et al., 2020). They suppress the immune response and reduce inflammation in the area around hair follicles. The best treatment for Central Centrifugal Cicatricial Alopecia (CCCA) depends on the stage and severity of the condition.
- Oral Anti-inflammatory Agents: Oral antibiotics, such as doxycycline, and anti-inflammatory drugs are used for more severe or widespread inflammation. Oral agents reduce deep follicular inflammation and pustules when topical treatments are insufficient (Vaughan et al., 2016). Oral agents are used in moderate to severe stages or when topical therapies are ineffective.
- Hair Growth Support: Minoxidil and platelet-rich plasma (PRP) stimulate hair regrowth and improve scalp health. Minoxidil helps in areas without scarring, and PRP shows promise in supporting hair follicle regeneration (Lehman et al., 2015). Recommended as adjunct therapy in early to moderate stages to enhance hair density.
- Hair Transplant: Surgical hair restoration involves transplanting healthy hair follicles to areas of the scalp that have been scarred or bald. Success depends on stable disease with no active inflammation, while outcomes vary but are effective for cosmetic improvement (Gathers et al., 2019). Healthy follicles are transplanted into areas where hair follicles are permanently destroyed.
- Antifibrotic or Hormonal Treatments: Emerging treatments include antifibrotic agents to reduce scarring and hormonal therapies to address underlying hormonal imbalances. Research is ongoing, as early studies suggest potential in slowing fibrosis and modifying disease progression (Olsen et al., 2020). The antifibrotic or hormonal treatments are considered the new treatment for CCCA alopecia.
- Lifestyle and Hair Care Modifications: Avoiding tight hairstyles, harsh chemicals, and heat treatments helps reduce mechanical and chemical scalp damage. Lifestyle and hair care modifications are crucial in preventing progression and reducing flare-ups (Gathers et al., 2019). It is recommended at all stages, especially for prevention and early management.
How Effective Is Hair Transplant for Treating CCCA?
Hair transplant is an effective solution for treating random bald spots caused by Central Centrifugal Cicatricial Alopecia (CCCA). A hair transplant is a viable option for patients once their medication has stabilized the disease and active inflammation has ceased, ensuring that hair loss no longer progresses. It works by harvesting healthy hair follicles from unaffected areas of the scalp and implanting them into the scarred, bald regions to restore hair density and improve appearance.
Turkey has become a popular destination due to its advanced medical facilities and affordable costs for patients considering a CCCA hair transplant. Vera Clinic is recognized as one of the best hair transplant clinics in Turkey, offering expert care, state-of-the-art technology, and personalized treatment plans. Patients benefit from experienced surgeons, high success rates, and comprehensive aftercare services.
Hair transplant remains a valuable option for patients with stable CCCA who seek to regain hair coverage. The procedure improves hair density and confidence. Exploring Hair Transplant Surgeries at reputable clinics, such as Vera Clinic in Turkey, offers access to high-quality care and effective outcomes for patients considering surgical solutions.
What to Expect Before and After a CCCA Hair Transplant
Before a CCCA hair transplant, patients must expect a thorough evaluation to confirm that the disease is inactive, as active inflammation leads to graft failure. Dermatologists require scalp biopsies and trichoscopy to assess disease activity. Medical management with anti-inflammatory treatments, such as corticosteroids or doxycycline, is prescribed for 6 to 12 months before considering surgery. A stable, scarred scalp with no signs of progression is essential for a successful transplant.
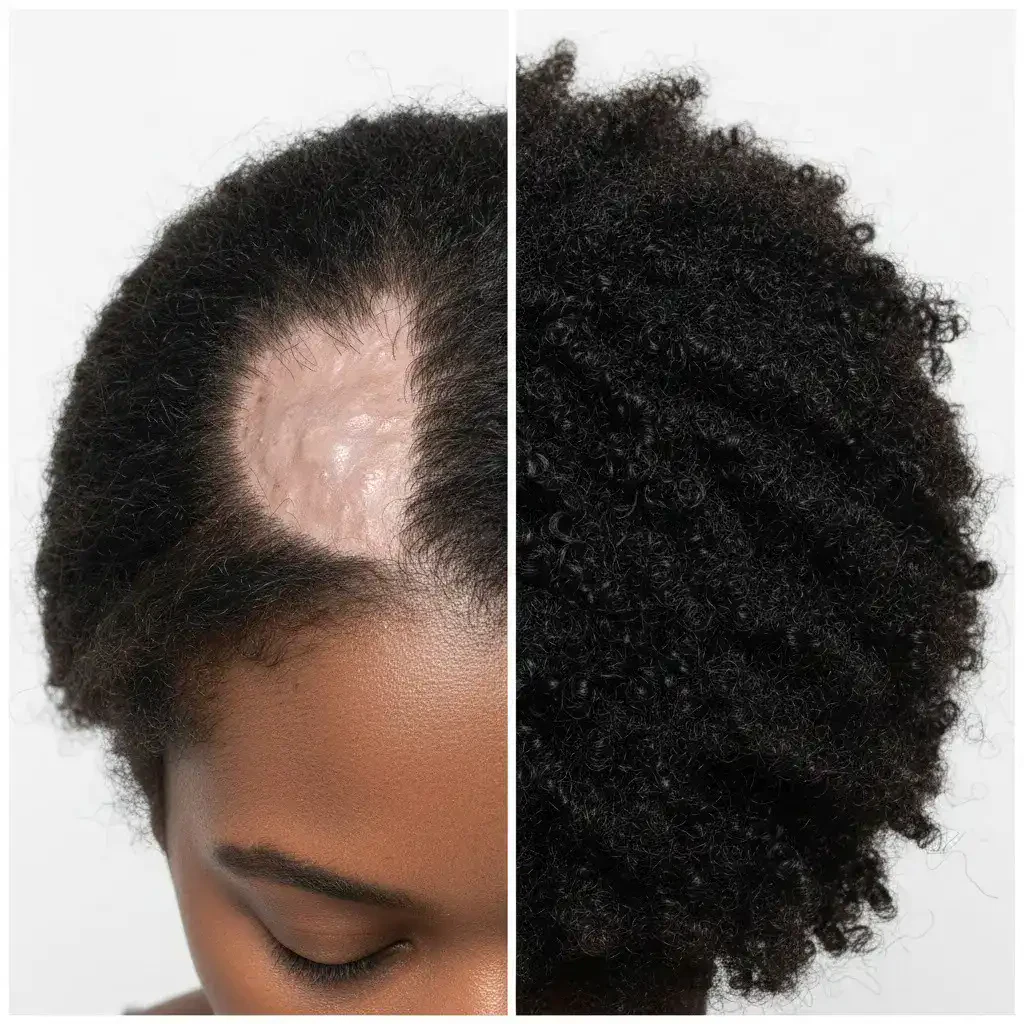
After a CCCA hair transplant, patients expect partial restoration of hair in affected areas, although outcomes vary depending on factors such as scar thickness, vascularity, and graft survival. Evidence shows that follicular unit transplantation (FUT) or follicular unit extraction (FUE) in CCCA cases has moderate success, with graft survival rates lower than in non-scarring alopecia. A 2016 study in the Journal of the American Academy of Dermatology reported that 60-80% of transplanted hairs survive in well-managed CCCA patients. Postoperative care includes anti-inflammatory maintenance to prevent recurrence and improve graft retention, and visual comparisons highlight the results through Hair Transplant Before After.
Before Centrifugal Cicatricial Alopecia hair transplant
After Centrifugal Cicatricial Alopecia hair transplant
When to See a Dermatologist for CCCA
See a dermatologist for CCCA as soon as symptoms of scalp inflammation and hair thinning appear, if the hair loss is progressive or accompanied by discomfort. Immediate medical attention is crucial when severe symptoms arise, such as persistent scalp redness, painful or tender areas, follicular pustules, significant patchy hair loss, or the development of smooth, shiny bald patches indicating scarring. The signs indicate active follicular destruction, which requires prompt treatment to prevent irreversible hair loss.
Early consultation with a specialist experienced in CCCA dermatology ensures accurate diagnosis and timely intervention, which slows or halts disease progression. Delaying medical care increases the risk of permanent scarring and irreversible hair loss, making early visits to a dermatologist essential for effective management and better outcomes.
How Is CCCA Diagnosed?
The procedures for diagnosing CCCA are listed below.
- Clinical Examination: Visual and tactile inspection of the scalp is used to detect central hair thinning, follicular dropout, perifollicular scaling, and scarring in the crown region. Signs such as breakage and reduced hair density appear, while advanced cases exhibit shiny, scarred skin in the early stages of CCCA. It is the first step in diagnosis and is essential for identifying the typical pattern of hair loss in CCCA.
- Trichoscopy: A non-invasive dermoscopic imaging tool used to magnify scalp and follicle structures. It reveals signs such as loss of follicular openings, perifollicular white-gray halos, hair shaft variability, and perifollicular erythema. It helps differentiate CCCA from other types of alopecia, like traction alopecia or lichen planopilaris. It is helpful during the early to moderate stages of disease to support Trichoscopy Diagnosis without the need for immediate biopsy.
- Scalp Biopsy: A 4mm punch biopsy is taken from an active margin of hair loss and sent for histopathologic analysis. Findings include perifollicular fibrosis, lymphocytic infiltrate, and destruction of the follicular epithelium. A biopsy is essential for confirming diagnosis, in unclear or atypical cases, or when treatment resistance occurs.
- Histological Stains: Special stains, such as Periodic Acid–Schiff (PAS), Elastic Van Gieson (EVG), or CD3 immunostaining, highlight fibrotic tissue, inflammatory cells, and basement membrane damage in CCCA. The stains provide a detailed evaluation of the severity of scarring and inflammation. They are used when routine histology does not yield a conclusive pattern or when a more in-depth analysis of inflammatory activity is required.
- Patient History: Detailed documentation of symptoms, family history, hair grooming practices, onset timing, and treatment history. CCCA is strongly linked to genetic factors and hairstyling practices, such as tight braids, weaves, and relaxers, making history essential to understanding its triggers and progression. The step is needed in all cases to guide clinical suspicion and rule out external causes of hair damage.
What Happens If You Are Diagnosed with CCCA Early Stages?
If you are diagnosed with CCCA in its early stages, immediate medical intervention slows progression, prevents permanent follicular scarring, and in some cases, promotes partial hair regrowth. Early-stage CCCA is characterized by perifollicular erythema, scaling, and hair thinning without extensive scarring, meaning hair follicles are not yet entirely destroyed and remain responsive to treatment. Early diagnosis enables dermatologists to initiate anti-inflammatory therapies before irreversible damage occurs.
Scientific research confirms the benefit of early detection and treatment. A study published in the Journal of the American Academy of Dermatology (Kyei et al., 2006) found that early initiation of therapy, including topical corticosteroids and oral tetracyclines like doxycycline, led to better outcomes in halting disease progression and preserving hair density. The findings underscore the value of early recognition and prompt intervention. Early diagnosis opens the door to potential regrowth with topical minoxidil, which has been used off-label to support hair regrowth in non-scarring alopecia and early scarring alopecia when follicles are still viable. Anti-inflammatory treatments, particularly intralesional corticosteroids and oral doxycycline, are more effective at controlling disease activity before fibrotic scarring develops.
The most effective treatments include anti-inflammatory agents, such as intralesional corticosteroids and oral doxycycline, combined with topical minoxidil, to encourage regrowth in cases where follicles remain intact during the early stages of CCCA. The therapies are most effective before significant fibrosis has set in, allowing for the preservation and stimulation of hair follicles.
What Happens If You Are Diagnosed with CCCA Late Stages?
If you are diagnosed with CCCA in the late stages, the hair loss is likely permanent in the affected areas due to advanced follicular destruction and scarring. Clinical signs include smooth, shiny scalp regions without follicular openings, indicating irreversible damage where hair follicles have been entirely replaced by fibrotic tissue in late-stage CCCA. Medical treatments are largely ineffective in restoring hair, but are still used to control residual inflammation and prevent progression to surrounding unaffected areas.
Scientific evidence highlights the limited efficacy of treatments once scarring has fully developed. Therapeutic interventions have minimal impact on regrowing hair in scarred regions once fibrosis is established, according to a study by Kyei et al. (2006) published in the Journal of the American Academy of Dermatology. Olsen et al. (2011) reported that late-stage CCCA patients experienced negligible hair recovery, even with aggressive medical therapy, reinforcing that the prevention of progression is the primary goal. Cosmetic solutions, such as wigs, hairpieces, or scalp micropigmentation, are commonly recommended for aesthetic restoration. Hair transplant is considered for selected patients if inflammation is completely inactive and the donor area is sufficient, though graft survival is lower in scarred tissue, and results are variable.
Suitable hair loss treatments include non-medical cosmetic options, such as wigs or scalp micropigmentation, for late-stage CCCA. Hair transplant is an option only if the disease is stable and inactive for at least 12 months. Outcomes are less predictable due to poor vascularity and scarring in the recipient area. Medical therapy remains supportive but is not curative at stage.
When Should You Take a Hair Consultation for CCCA?
You should take a hair consultation for CCCA when there is early thinning at the crown, persistent scalp tenderness, itching, or a burning sensation, as the symptoms are initial signs of inflammation that lead to permanent follicular damage. Severe symptoms such as patchy hair loss, perifollicular scaling, and shiny, scarred scalp areas without visible hair follicles indicate active and potentially scarring alopecia as the condition worsens. A consultation becomes critical at stage to perform scalp analysis, trichoscopy, and possibly a biopsy to confirm diagnosis and begin treatment. Research from the Journal of the American Academy of Dermatology (Kyei et al., 2006) indicates that early intervention is crucial in halting disease progression and preserving hair follicles. A Hair Transplant Consultation is required to evaluate options for surgical restoration after inflammation is fully controlled, when the disease is diagnosed late, or hair loss is extensive.
Does Hair Regrowth when Central Centrifugal Cicatricial Alopecia Is Treated in Its Late Stages?
Hair regrowth does not occur when Central Centrifugal Cicatricial Alopecia (CCCA) is treated in its late stages because the hair follicles are permanently destroyed and replaced with scar tissue. The scalp appears smooth and shiny, indicating the loss of follicular openings, which makes regrowth biologically impossible in smooth and shiny areas in late-stage CCCA. Treatment at the late stage focuses on halting further progression rather than restoring lost hair.
Research published in the Journal of the American Academy of Dermatology (Kyei et al., 2006) confirms that early diagnosis and treatment are critical in preventing irreversible follicular scarring. Anti-inflammatory therapies, such as intralesional corticosteroids and doxycycline, help control the disease and allow for regrowth when inflammation is present but follicles are still partially intact. Olsen et al. (2011) further demonstrated that early-stage CCCA patients maintained better hair density and responded more favorably to treatment compared to patients in advanced stages of the disease.
Central Centrifugal Cicatricial Alopecia treatment causes hair regrowth only during early stages, when inflammation is active but scarring is minimal and follicles are still viable.
How Do Vitamins Help Hair Growth in CCCA Hair Loss?
Vitamins help support hair growth in CCCA hair loss by improving scalp health, improving follicular function, and correcting nutritional deficiencies that may exacerbate thinning during the early stages of the disease. Maintaining adequate levels of specific vitamins strengthens the scalp environment and complements medical treatments, though CCCA is primarily a scarring inflammatory condition.
Vitamin D is one of the most essential nutrients for regulating hair follicles, and low levels have been associated with multiple types of alopecia, including scarring forms. A study published in the International Journal of Dermatology (Rasheed et al., 2013) found significantly lower vitamin D levels in women with hair loss compared to control subjects. Biotin plays a crucial role in maintaining keratin infrastructure and is beneficial in cases of proven deficiency, although it is not effective when levels are normal. Iron is vital because low ferritin has been linked to chronic diffuse hair loss, and restoring ferritin above 70 ng/mL is recommended in hair loss protocols. Zinc is essential for maintaining immune balance and promoting follicle recovery in the presence of inflammation.
Supplementation is recommended only when deficiencies are confirmed through blood tests. Over-supplementation with vitamin A or zinc leads to toxicity or exacerbates hair shedding. Medical supervision is essential for tailoring supplementation to each patient’s specific needs and preventing unnecessary or harmful intake. The best vitamins for CCCA alopecia include vitamin D, iron (ferritin), zinc, and biotin; however, their use is guided by professional evaluation and lab-based testing.
How Does CCCA Differ from Other Types of Hair Loss?
Central Centrifugal Cicatricial Alopecia (CCCA) differs from other types of hair loss by being a form of scarring alopecia, which leads to the permanent destruction of hair follicles and their replacement with fibrous (scar) tissue. The irreversible damage sets it apart from non-scarring types of hair loss, where hair follicles remain intact and regrowth is possible. CCCA starts at the crown or vertex of the scalp and expands outward in a symmetrical pattern. It is commonly seen in women of African descent and is associated with genetic predisposition and damaging hair practices such as tight braids and chemical relaxers. CCCA involves chronic inflammation that leads to irreversible hair loss if left untreated, unlike non-scarring forms of hair loss.
Trichotillomania is a behavioral disorder characterized by the patient pulling out their hair, resulting in irregular bald patches with broken hairs of varying lengths. Alopecia universalis is an autoimmune condition characterized by the complete loss of hair on the scalp and body, without scarring, which allows for the possibility of regrowth with appropriate treatment. Traction alopecia is caused by prolonged tension on hair follicles, resulting from hairstyles that pull tightly, and is reversible if diagnosed early before follicular scarring occurs. Tinea capitis causes patchy hair loss, accompanied by scaling, inflammation, or black dots, and is effectively treated with antifungal medications. Scarring alopecia includes CCCA and other variants, such as lichen planopilaris or frontal fibrosing alopecia, all of which cause permanent hair loss due to follicular destruction and fibrosis. Understanding the distinctions is important when comparing different hair loss types.
The overview comparison of different types of Hair Loss is shown in the table below.
| Type | Cause | Pattern | Reversibility |
|---|---|---|---|
| Central Centrifugal Cicatricial Alopecia | Inflammatory scarring, hair trauma, and genetics | Symmetrical crown-centered thinning | Irreversible if untreated |
| Trichotillomania | Behavioral (hair-pulling disorder) | Irregular patches with broken hairs | Reversible if stopped early |
| Alopecia Universalis | Autoimmune | Complete scalp and body hair loss | Potentially reversible with treatment |
| Traction Alopecia | Mechanical tension from hairstyles | Frontal or marginal thinning | Reversible if tension is eliminated early |
| Tinea Capitis | Fungal infection | Patchy hair loss with scaling or pustules | Reversible with antifungal treatment |
| Scarring Alopecia (General) | Inflammatory or autoimmune destruction | Variable based on subtype | Generally irreversible once scarred |
How Is Central Centrifugal Cicatricial Alopecia Different from Lichen Planopilaris?
Central Centrifugal Cicatricial Alopecia is different from Lichen Planopilaris in terms of cause, clinical features, histopathology, and patient demographics. CCCA is most commonly linked to genetic predisposition and physical or chemical trauma to the scalp in women of African descent. It starts at the crown of the scalp and spreads outward in a circular pattern. Lichen Planopilaris is an autoimmune disorder characterized by T-cell–mediated inflammation that targets hair follicles, presenting as patchy hair loss accompanied by perifollicular redness and scaling, which eventually leads to scarring.
CCCA presents with central scalp thinning, tenderness, or burning, without significant visible redness in early stages. LPP is marked by perifollicular scaling, itching, and a more random patchy distribution across the scalp. CCCA features concentric lamellar fibrosis and premature desquamation of the inner root sheath. LPP shows a lichenoid lymphocytic infiltrate at the follicular infundibulum and isthmus, with hypergranulosis and a sawtooth pattern of the outer root sheath.
A study published in the Journal of the American Academy of Dermatology (Olsen et al., 2011) emphasizes these distinctions in the immunopathologic profiles and the typical demographics affected. CCCA overwhelmingly affects African American women between 30 and 55 years old, while LPP has a broader demographic reach and is common in postmenopausal Caucasian women.
Understanding the clinical and histological differences between these two conditions is essential for accurate diagnosis and appropriate treatment. The conditions fall under the category of scarring alopecias but follow very different mechanisms. One is primarily inflammation and trauma-induced, while the other is autoimmune. The differences are crucial when evaluating scarring alopecias, such as Lichen Planopilaris.
How Is Central Centrifugal Cicatricial Alopecia Ariata Different from Alopecia ?
Central Centrifugal Cicatricial Alopecia is different from Alopecia Areata based on cause, clinical presentation, and disease progression. CCCA is a type of scarring alopecia primarily caused by chronic inflammation and mechanical or chemical trauma to the scalp. It leads to permanent hair loss as it destroys hair follicles and replaces them with fibrous tissue. Hair loss begins at the crown and spreads outward in a circular pattern. Alopecia areata is an autoimmune condition in which the immune system mistakenly attacks hair follicles, causing sudden, non-scarring, patchy hair loss that can occur on the scalp, face, or body. The follicles remain intact, allowing for the potential of spontaneous regrowth.
CCCA progresses slowly and irreversibly if left untreated, presenting symptoms such as burning, tenderness, or scalp discomfort. Alopecia areata progresses unpredictably, sometimes resolving completely without treatment or advancing to total loss of scalp or body hair. A study published in the Journal of the American Academy of Dermatology (Olsen et al., 2011) distinguishes CCCA as a chronic scarring condition. Alopecia Areata is a non-scarring condition that presents in episodic form. The distinction between cicatricial alopecia vs alopecia areata is essential for appropriate diagnosis and management strategies. The conditions require different treatment approaches, with immunomodulatory therapies commonly used in Alopecia Areata.