Dialysis can causes hair loss in some patients. Hair thinning and shedding are recognized side effects in some patients undergoing long-term dialysis. This happens because dialysis filters waste from the blood and places stress on the body, which disrupts hair growth cycles.
Dialysis hair loss is a type of secondary hair loss linked to medical treatment rather than genetics. It often shows up as diffuse thinning across the scalp rather than isolated bald patches.
The connection between dialysis and hair loss is tied to multiple factors: nutritional deficiencies (such as low zinc, folate, or protein), chronic illness stress, changes in blood circulation, and certain medications prescribed during treatment. Over time, these factors weaken the hair follicles, causing increased shedding and slower regrowth.
In clinical terms, dialysis hair loss is classified under treatment-related alopecia, which means it occurs as a consequence of the therapy itself rather than a primary scalp disorder. While not universal, many patients report noticeable thinning, especially after months or years of treatment, making it an important quality-of-life issue in kidney care.
How Does Dialysis Make You Lose Your Hair?
Hair loss is a reported complication of dialysis, though not every patient experiences it. The process itself, along with the underlying chronic kidney disease (CKD), both contribute to thinning and shedding. The distinction is important: dialysis indirectly triggers changes that affect hair health, but CKD already places stress on the body and its metabolic balance.
The mechanisms behind hair loss in dialysis are multifactorial rather than caused by a single pathway. Dialysis alters protein, vitamin, and mineral levels, which weakens follicle metabolism. Medications such as anticoagulants and phosphate binders have hair loss listed as potential side effects. The stress of long-term illness also shifts hair follicles into the telogen (resting) phase, producing diffuse shedding across the scalp.
Alopecia is significantly more common in dialysis patients compared to healthy controls, with diffuse hair thinning being the most typical presentation according to “Diffuse alopecia in a hemodialysis patient caused by a low-molecular-weight heparin, tinzaparin” by Sarris et al., Am J Kidney Dis. The study highlighted nutritional imbalance, uremic toxins, and treatment stress as contributing factors.
How Do Uremic Toxins Contribute to Hair Shedding During Dialysis?
Uremic toxins are nitrogenous wastes and other metabolites (small, middle, and protein-bound solutes such as indoxyl sulfate and p-cresyl sulfate) that accumulate when kidneys fail and are not fully cleared between dialysis sessions. Protein-bound toxins, in particular, are poorly removed by standard hemodialysis, so levels remain elevated and fluctuate, stressing tissues between runs.
These toxins drive oxidative stress and inflammation; mechanisms known to impair hair-follicle cells. Indoxyl sulfate increases reactive oxygen species and depletes antioxidant defenses (glutathione), disrupting cellular metabolism; such redox imbalance hinders dermal papilla and matrix cell function that supports anagen growth according to “The uremic solute indoxyl sulfate induces oxidative stress in endothelial cells” published in Journal of Thrombosis and Haemostasis.
Because clearance is incomplete (especially for protein-bound solutes), toxins re-accumulate between treatments, promoting a shift of follicles into telogen (shedding phase) and contributing to diffuse thinning rather than patchy loss; clinically, dialysis and advanced CKD populations show higher rates of hair changes and telogen effluvium than the general population.
Mechanistic studies consistently link indoxyl sulfate to oxidative and inflammatory signaling across human cells (endothelial, immune, and others), offering a biologic pathway for follicle stress in uremia even if direct follicle-cell trials are limited. Reviews and experiments document IS-induced ROS generation and antioxidant depletion, and they highlight poor dialytic removal of protein-bound toxins as a persistent exposure source.
Why Does Telogen Effluvium Occur in People Undergoing Dialysis?
In patients on dialysis, the physiological stresses (metabolic fluctuations, toxin accumulation, nutritional deficiencies, and ongoing systemic illness) act as triggers that push follicles into the telogen phase earlier than they normally would. The stress of dialysis and underlying chronic kidney disease (CKD) accelerates this shift.
Typically, the diffuse shedding from telogen effluvium appears 2–3 months after the triggering event; so many people on dialysis begin noticing increased hair shedding a few months into treatment.
Although dialysis worsens or precipitates TE, the underlying CKD itself plays a major role in causing metabolic imbalance, uremic toxin buildup, hormonal irregularities, and nutrient deficiencies. The result is that dialysis and CKD contribute jointly, through multiple pathways, not a single isolated cause. (Telogen Effluvium: A Review by Shashikant Malkud published in Journal of Clinical and Diagnostic Research)
Is Anagen Effluvium a Possible Complication of Dialysis Treatment?
Anagen effluvium is hair loss that occurs when follicles in the active growth (anagen) phase are abruptly damaged, usually by toxins, chemotherapy, or radiation. Unlike telogen effluvium, which involves a shift into the resting phase, anagen effluvium represents direct follicular injury.
In dialysis patients, this condition is less common but still possible. Uremic toxins and oxidative stress impair rapidly dividing hair-matrix cells, leading to fragility and breakage of shafts still in the growth phase. Certain medications used in kidney disease (such as immunosuppressants after transplantation or high-dose anticoagulants) contribute to anagen-type shedding.
Toxic accumulation in chronic kidney disease and oxidative stress during dialysis theoretically trigger anagen effluvium, though cases are rarer compared to telogen effluvium, which remains the predominant form of dialysis-related alopecia according to“Cutaneous Manifestations of Chronic Kidney Disease” (Indian Dermatology Online Journal, 2021)
Thus, while dialysis hair loss most often presents as diffuse telogen shedding, anagen effluvium remains a potential, albeit less frequent, complication tied to the toxic environment of advanced kidney disease and its treatment.
How Do Nutritional Deficiencies Affect Hair in Dialysis Patients?
Nutritional deficiencies in dialysis patients weaken hair growth because these patients often follow strict dietary restrictions (on protein, potassium, phosphorus) and suffer malabsorption or loss of micronutrients during dialysis.
Deficits in iron, zinc, protein, B vitamins (B6, B9, B12), and vitamin D are especially harmful. Iron deficiency impairs oxygen delivery to follicle cells. Zinc is essential for DNA synthesis and enzyme function. Protein provides the amino acids keratin and collagen. B vitamins support cellular metabolism in hair matrix cells. Vitamin D regulates follicle cycling via the vitamin D receptor in keratinocytes. (The Role of Vitamins and Minerals in Hair Loss: A Review)
Supplementation in dialysis follows renal-safe guidelines: standard “renal vitamins” including B complexes and vitamin D analogs (not excessive doses) are prescribed, guided by blood tests, to prevent toxicity or unwanted accumulation.
Zinc, selenium, and other trace elements are significantly depleted in dialysis patients compared to healthy subjects according to “Trace Elements and Their Management in Dialysis Patients” (Wakino et al., 2023), highlighting how mineral loss affects multiple systems including hair.
Can High Phosphorus Cause Hair Loss?
High phosphorus does not directly cause baldness, but in dialysis patients hyperphosphatemia disrupts mineral balance and hormones, which can weaken follicles and contribute to diffuse hair thinning.
Why Is Erythropoietin Deficiency Linked to Hair Thinning in Dialysis Patients?
Erythropoietin (EPO) is best known for stimulating red blood cell production, but it also supports microvascular function and tissue health, including scalp circulation. In dialysis patients, EPO deficiency worsens anemia, reducing scalp oxygen delivery and impairing follicle metabolism and growth.
Studies show stronger anemia correlates with greater hair thinning in chronic kidney disease: patients with lower hemoglobin levels often report more diffuse hair loss alongside other uremic symptoms. (Medscape reports that hair changes are common in CKD and dialysis populations.
While direct trials specifically linking EPO deficits to hair follicle apoptosis are rare, the combination of poor oxygenation, oxidative stress, and metabolic strain in EPO-deficient states provides a plausible pathway for thinning in dialysis patients.
How Does Secondary Hyperparathyroidism Impact Hair Growth During Dialysis?
Secondary hyperparathyroidism (SHPT) is a condition in chronic kidney disease wherein the parathyroid glands secrete excess parathyroid hormone (PTH) in response to low calcium, high phosphate, and reduced active vitamin D.
Elevated PTH disrupts calcium and phosphorus balance: it pulls calcium from bones, increases renal phosphate excretion (impaired in CKD), and stimulates vitamin D activation, all of which become maladaptive in kidney failure.
When PTH and mineral imbalance persist, hair structure weakens: calcium imbalance reduces keratinocyte cohesion, high phosphate salts deposit and interfere with follicular microenvironments, and ongoing metabolic stress leads follicles to produce weaker, brittle strands. Follicles under mineral stress shrink (miniaturize) or enter rest prematurely.
How Does Oxidative Stress During Dialysis Damage Hair Follicles?
Oxidative stress occurs when reactive oxygen species (ROS) overwhelm a follicle’s antioxidant defenses, damaging DNA, lipids, and proteins essential for healthy growth. The imbalance disrupts the hair growth cycle by pushing follicles prematurely into catagen or telogen, reducing anagen phase duration and causing thinning.
In dialysis patients, increased oxidative load from uremic toxins, inflammation, and repeated blood–membrane interactions intensifies ROS exposure. This stress weakens follicular stem cells, impairs dermal papilla signaling, and accelerates follicle miniaturization, making hair thinner and more fragile.
ROS interfere with signaling pathways like Nrf2/ARE, MAPK, and NF-κB; pathways essential for follicle cell survival and regeneration according to “Oxidative stress in hair follicle development and hair growth”.
Can Oxidative Stress Accelerate Hair Loss in Patients Undergoing Dialysis?
Yes, oxidative stress can accelerate hair loss in dialysis patients by increasing free radicals, which damage follicular cells and trigger early apoptosis or aging-like changes.
During dialysis, repeated blood contact with artificial membranes, reperfusion cycles, inflammation, and uremic toxin overload generate excess reactive oxygen species (ROS). This oxidative burden overcomes the follicle’s antioxidant defenses, causing cellular damage and pushing follicles out of the growth phase prematurely.
ROS disrupts key signaling pathways (like Nrf2, MAPK, NF-κB) and induce apoptosis or senescence in hair follicle cells according to “Oxidative stress in hair follicle development and hair growth”.
How Does Microvascular Ischemia Affect Follicle Health in Dialysis Patients?
Microvascular ischemia means the hair follicles receive poor, inadequate blood flow due to damage or narrowing of the small vessels supplying them.
In dialysis patients, factors like anemia (low red blood cells), vascular calcification, and hypotensive episodes during sessions reduce microcirculatory perfusion in the scalp. These conditions lead to low perfusion, meaning follicle cells get insufficient oxygen, nutrients, and waste removal; stress that weakens the follicle, shortens its growth phase, or causes miniaturization and shedding.
Which Patients Are Most at Risk of Hair Loss During Dialysis?
Patients most at risk include those who are elderly, on long-term dialysis, malnourished, female, or with autoimmune comorbidities. Those taking multiple medications also face higher risk due to drug interactions and added systemic stress.
Alopecia affects about 10% of dialysis patients with a broader 25–38% reporting hair changes according to “Alopecia in Renal Disease: Common and Troublesome, but Treatable” published in Medscape.
How Does Dialysis Treatment Contribute to Hair Loss in Kidney Failure?
Hair loss is a reported complication of dialysis, though it does not affect every patient. In people with chronic hair loss kidney disease (CKD), both the underlying disease and dialysis treatment combine via multiple pathways to worsen hair thinning; so it’s not just one cause at play.
Dialysis contributes indirectly by inducing oxidative stress, fluctuations in nutrient and mineral levels, episodes of low blood pressure, and removal or loss of essential micronutrients. Meanwhile, CKD and hair loss itself causes uremic toxin accumulation, hormonal imbalances, anemia, and malnutrition; factors that predispose to hair shedding even before dialysis begins.
Dialysis patients had significantly higher rates of diffuse hair thinning and brittle hair (77.6% and 69.0%, respectively) according to “From Luster to Loss: The Impact of Chronic Kidney Disease on Hair Health,” compared to non-dialysis CKD hair loss patients, supporting the idea that dialysis amplifies hair-related complications.
Does Kidney Failure Cause Hair Loss?
Yes, kidney failure causes hair loss because advanced CKD disrupts multiple systems essential for follicle health. Uremic toxin buildup, anemia from erythropoietin deficiency, mineral imbalances (calcium, phosphorus, vitamin D), and chronic inflammation all interfere with the hair growth cycle, often leading to diffuse thinning rather than patchy baldness.
Over 70% of dialysis patients experience hair changes, including shedding and brittle texture according to “From Luster to Loss: The Impact of Chronic Kidney Disease on Hair Health,” linking CKD’s metabolic and hormonal disturbances directly to alopecia.
CKD hair loss is a well-recognized complication of kidney failure, reflecting the body’s systemic stress rather than a scalp-only disorder.
What Types of Dialysis Are Most Likely to Cause Hair Loss?
Hemodialysis is the type of dialysis most often implicated in hair loss. Because it involves intermittent filtering of large blood volumes through artificial membranes, it produces stronger fluctuations in fluid balance, nutrient levels, oxidative stress, and blood pressure, all of which heighten follicle stress.
This modality is commonly used in patients with end-stage kidney disease (ESKD), especially for those who cannot perform or tolerate peritoneal dialysis. In the literature, case reports link hair loss to hemodialysis patients; e.g. a 47-year-old man began systemic hair loss one month after starting hemodialysis, likely linked to endothelial capillary regression. (“Hair Loss in a Hemodialysis Patient after Repetitive Use of the Antipruritic Drug Nalfurafine: Implications of Impaired Angiogenesis for Hair Loss”)
In contrast, peritoneal dialysis tends to cause less acute systemic fluctuations, making it somewhat less likely to trigger hair shedding directly. Nonetheless, underlying chronic kidney disease (CKD) means any dialysis modality contributes to hair loss through shared systemic pathways.
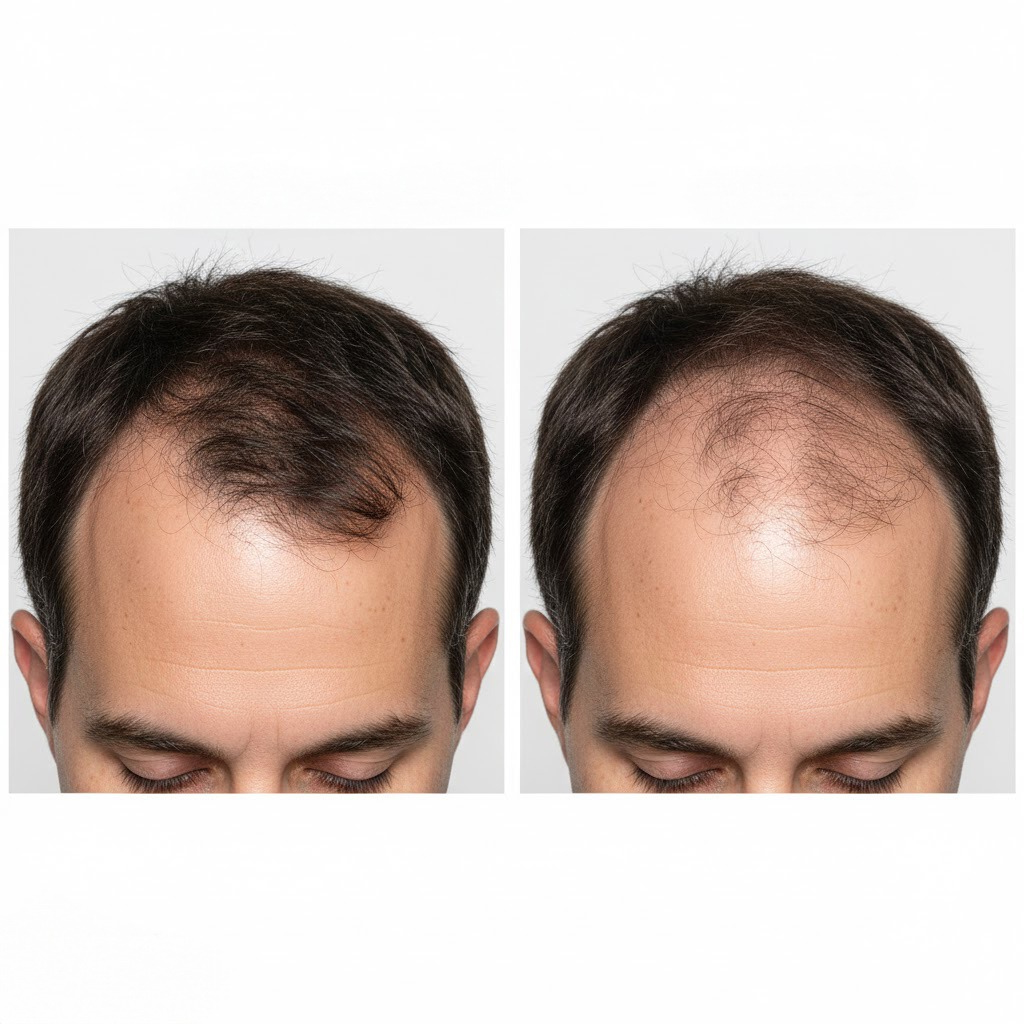
What Does Hair Look Like Before and After Dialysis Hair Loss?
Before dialysis hair loss, hair appears fuller and denser, while after it often looks thinner, weaker, and more brittle across the scalp.
How to Stop Hair Loss from Dialysis
Dialysis hair loss treatment focuses on addressing the underlying causes (nutritional deficiencies, anemia, hormonal imbalance, oxidative stress, and medication side effects) rather than the dialysis process alone. While results vary, consistent treatment often improves shedding within 3–6 months, with fuller recovery possible in 6–12 months depending on patient health and severity.
- Nutritional Supplementation: Corrects deficits in iron, zinc, protein, B vitamins, and vitamin D that are common in dialysis. Supplements improve follicle strength and regrowth, with noticeable results in 3–6 months when deficiencies are resolved.
- Erythropoietin (EPO) Therapy: Treats anemia by restoring red blood cell levels, improving scalp oxygenation, and reducing thinning linked to low hemoglobin. Effective in most dialysis patients once hemoglobin stabilizes.
- Phosphate and Calcium Control: Managing phosphorus with binders and regulating parathyroid hormone reduces follicle stress from mineral imbalance, lowering brittle hair risk over time.
- Antioxidant Support: Vitamin E, C, or N-acetylcysteine limit oxidative stress in follicles; studies show reduced cell damage, but clinical hair regrowth varies by patient.
- Medication Adjustment: Switching or lowering doses of drugs known to trigger shedding (such as certain anticoagulants or immunosuppressants) stop progression, with regrowth starting within a few months.
- Topical and Dermatologic Therapies: In select patients, minoxidil or PRP therapy is used to stimulate regrowth; these are considered when conservative measures fail and are monitored by dermatologists.
- Hair Transplantation: Rarely, for patients with stable kidney disease and persistent loss, surgical options are considered. This is usually a last resort after systemic issues are corrected.
What Are the Best Vitamins for Hair Loss from Dialysis?
The best vitamins for dialysis hair loss are those that support follicle metabolism, red blood cell function, and overall cell repair, since dialysis patients often face malabsorption and dietary restrictions. Each vitamin plays a crucial role in maintaining follicle survival and stimulating regrowth.
- Vitamin D: Essential for calcium balance and follicle cycling; deficiency is common in dialysis and strongly linked to diffuse thinning. Vitamin D receptors regulate hair follicle activity, making supplementation vital for restoring normal growth.
- Vitamin B12: Supports DNA synthesis and red blood cell formation. In dialysis patients, low B12 contributes to anemia and poor scalp oxygenation, which accelerates shedding. Correcting B12 deficiency helps both systemic energy and follicle regrowth.
- Biotin (Vitamin B7): Strengthens keratin structure and improves hair shaft resilience. Although biotin deficiency is rare, dialysis impairs absorption, and supplementation often enhances hair texture and reduces brittleness.
- Folic Acid (Vitamin B9): Works with B12 in DNA synthesis and red blood cell production. Adequate folate is critical in dialysis patients to improve blood quality and nutrient delivery to follicles.
- Vitamin C: Functions as an antioxidant, protecting follicles from oxidative stress during dialysis. It also enhances iron absorption, improving red blood cell levels and scalp oxygenation.
- Vitamin E: Another strong antioxidant that reduces free radical–induced follicle damage common in dialysis. Supplementation supports healthier scalp circulation and prevents premature follicle aging.
- Vitamin A: Helps regulate sebum production, which maintains scalp hydration. However, excess intake worsens hair loss, so careful monitoring is required in dialysis patients.
- Vitamin K: Supports vascular health and prevents calcification of small blood vessels, improving follicle blood flow in chronic kidney disease patients.
How Effective Is Hair Transplant for Treating Dialysis Permanent Hair Loss?
Hair transplant is a viable solution for permanent hair loss in dialysis patients; especially when shedding has stabilized and underlying medical issues are controlled. Because transplant success relies on healthy donor follicles and sufficient blood supply, it should only be considered after nutritional, hormonal, and medication-related hair losses are addressed.
The procedure is recommended for dialysis patients when:
- Hair loss has plateaued and shows no further decline over 12 months,
- Anemia, vitamin deficiencies, and metabolic imbalances are corrected,
- Donor hair quality and density remain adequate,
- The patient’s overall health is stable and dialysis regimen is predictable.
Many patients choose to have a hair transplant in Turkey, which offers high medical standards, competitive pricing, and experience in hair restoration surgery. Vera Clinic stands out as one of the top choices in Turkey due to its combination of cutting-edge techniques, strong survival rates, and comprehensive aftercare programs tailored for patients with medical comorbidities.
What to Expect Before and After a Hair Transplant for Dialysis Hair Loss?
Before a hair transplant for dialysis hair loss, patients undergo medical evaluation to ensure stable kidney function, corrected anemia, and adequate donor hair availability.
After the transplant, graft survival and natural regrowth are generally successful if systemic health is well managed, with visible improvements starting at 3–4 months and maturing by 12 months.
Check the hair transplant before and after pictures below!
How is Dialysis Hair Loss Diagnosed?
It is diagnosed through scalp examination, patient history, and exclusion of other causes like thyroid or drug-induced alopecia. Hair transplant consultation helps you to diagnose your issue.
When to See a Dermatologist for Hair Loss due to Dialysis?
Seek medical care if you notice sudden shedding, bald patches, scalp infection signs, or progressive thinning despite treatment.
How Long Does It Take for Hair to Regrow After Dialysis?
Hair regrowth after dialysis-related shedding typically takes 3–6 months, with many patients reporting visible thickening by the 6–9 month mark once nutritional and metabolic balance is restored. Studies show that around 60–70% of dialysis patients with telogen effluvium recover partial density within 6 months, while full regrowth takes up to 12 months, depending on factors like anemia control, phosphorus balance, and overall health. Permanent regrowth is limited in cases where chronic kidney disease or oxidative stress causes lasting follicle damage.
How to Prevent Hair Loss While Undergoing Dialysis Therapy
Preventing hair loss during dialysis therapy requires a proactive approach that combines medical management, nutritional support, and gentle hair care practices.
- Optimize Nutritional Status: Work with a renal dietitian to ensure adequate intake of protein, iron, zinc, B vitamins, and vitamin D while respecting dialysis dietary limits.
- Treat and Monitor Anemia Proactively: Use erythropoietin or iron supplementation to maintain hemoglobin in target ranges, ensuring proper oxygen delivery to scalp follicles.
- Control Mineral Imbalances: Keep phosphorus, calcium, and PTH levels within recommended ranges to reduce follicle stress caused by secondary hyperparathyroidism.
- Antioxidant Support: Under medical supervision, consider safe antioxidants (vitamins C, E, N-acetylcysteine) to reduce oxidative stress on follicles.
- Gentle Hair Care: Use mild shampoos, avoid tight hairstyles or friction, and limit heat styling or aggressive chemical treatments.
- Medication Review: Ask your nephrologist to evaluate medications that might aggravate hair shedding (e.g. certain anticoagulants or immunosuppressants) and adjust if possible.
- Optimize Dialysis Regimen: Minimize hypotensive episodes, ensure adequate dialysis adequacy (Kt/V), and use biocompatible dialysis membranes to reduce inflammatory and oxidative burden.
- Monitor Scalp Health: Check regularly for signs of scalp infection, folliculitis, or inflammation and seek early dermatologic care if needed.
- Manage Comorbidities: Control diabetes, thyroid disorders, and autoimmune conditions, as they compound hair loss risk.
- Regular Dermatology Assessment: Involve a dermatologist early—especially if hair thinning begins—to track regrowth, start topical therapies, or intervene before follicle loss becomes permanent.
A 2015 observational study in Renal Failure observed that dialysis patients with well-controlled anemia and nutrition had significantly lower rates of diffuse hair thinning, suggesting that system-wide optimization helps reduce hair loss in this population.