Lamotrigine, sold under the brand name Lamictal, is a medication primarily prescribed as a mood stabilizer and anticonvulsant. It is widely used in the management of bipolar disorder or BPD (borderline personality disorder) especially for preventing depressive episodes, and is sometimes used off-label as an adjunct antidepressant treatment. Unlike many mood-stabilizing drugs, lamotrigine is often valued for its relatively mild side-effect profile, particularly in long-term therapy.
Lamotrigine is effective in reducing the frequency and severity of depressive episodes in bipolar and borderline patients. It is less effective for acute mania, but its utility in mood stabilization makes it a cornerstone treatment for individuals who experience recurring depression. Many psychiatrists consider lamotrigine a safer maintenance therapy than alternatives that induce weight gain, sedation, or metabolic side effects.
Although uncommon, lamotrigine hair loss is a reported side effect which means lamotrigine causes hair loss. This condition refers to diffuse or patchy shedding that occur while taking the medication. The link between lamictal and hair loss is believed to stem from mechanisms such as drug-induced telogen effluvium (forcing hair prematurely into the resting/shedding phase) or nutrient depletion caused by long-term use. Hair loss is reversible if the dose is adjusted or the medication is discontinued, but recurrence is possible if therapy continues according to the reported cases “Alopecia in association with lamotrigine use: an analysis of individual case safety reports in a global database” published in Drug Safety).
Lamictal hair loss is an uncommon but recognized side effect, and patients experiencing shedding should consult their prescribing doctor to discuss dosage adjustments, supplementation, or alternative therapies.
How Common is Hair Loss in People Taking Lamotrigine?
Hair loss in people taking lamotrigine (Lamictal) is considered uncommon, but it has been consistently reported in post-marketing safety databases and case reports. Clinical trial data do not provide a precise percentage, but pharmacovigilance studies suggest it occurs in a small minority of users.
337 cases of alopecia were reported with lamotrigine up to April 2009, with many improving after dose reduction or discontinuation in a study titled “Alopecia in Association with Lamotrigine Use: An Analysis of Individual Case Safety Reports in a Global Database” (Drug Safety, 2010).
A total of 1,656 reports of alopecia linked to antiseizure medications were compiled, with 355 associated with lamotrigine, ranking hair loss due to medication and this drug behind valproate but among the more frequently reported agents according to “Antiseizure Medication-Induced Alopecia: A Literature Review” (Brain Sciences, 2023).
While exact population risk is unknown, available data indicate lamotrigine-related hair loss is rare (likely <1%), but real. It is generally reversible once the medication is stopped or adjusted.
Why Is Hair Loss a Side Effect of Lamotrigine (Lamictal)?
Hair loss is a side effect of Lamotrigine (Lamictal) because the drug alters follicular cycling, triggers telogen effluvium through metabolic stress, and interferes with nutrient absorption essential for hair growth in some patients. The mechanism behind lamotrigine side effects hair loss involves disruption of keratinocyte function, mitochondrial stress in follicular cells, and immune-mediated reactions that weaken the hair shaft.
In some cases, lamotrigine causes trace element deficiencies (zinc, selenium) that are critical for follicle integrity. Lamictal side effects hair loss is thought to arise from a combination of direct follicular toxicity and secondary metabolic imbalance according to “Antiseizure Medication-Induced Alopecia: A Literature Review” (Brain Sciences, 2023), making it one of the better-documented but underrecognized adverse effects.
Does Lamotrigine Make Your Hair Fall Out?
Yes. Lamotrigine makes your hair fall out as a seldomly reported side effect, most commonly in the form of telogen effluvium. This happens because lamotrigine disrupts hair follicle cycling, impairs keratinocyte activity, and creates trace element imbalances such as zinc and selenium deficiencies that are critical for follicle health.
Can Anagen Effluvium Be a Side Effect of Lamotrigine?
Yes, but rarely. Anagen effluvium can occur as a side effect of lamotrigine, though it is far less common than telogen effluvium. Anagen effluvium is thought to result from direct toxic or oxidative stress on rapidly dividing follicular matrix cells during the active growth phase of hair.
How Does Lamotrigine Cause Hair Loss?
Lamotrigine causes hair loss by disrupting the normal hair growth cycle, most often through telogen effluvium, where follicles prematurely shift into the resting phase. The medication has been linked to alterations in keratinocyte function, micronutrient imbalances (such as zinc and selenium depletion), and increased cellular stress responses that impair follicle metabolism. In some cases, lamotrigine indirectly triggers hair shedding through hormonal and stress-related changes that disturb scalp homeostasis.
Beyond these mechanisms, researchers note that lamotrigine creates oxidative stress within rapidly dividing hair matrix cells, contributing to follicular miniaturization or, more rarely, anagen effluvium.
How Long Does it Take for Lamotrigine to Cause Hair Loss?
Hair loss from lamotrigine typically develops within the first 2–6 months of treatment, but timing varies depending on dosage, genetics, and individual sensitivity.
When Does Hair Loss Usually Start After Taking Lamotrigine?
Hair loss usually begins within 2–6 months after starting lamotrigine, as the drug shifts follicles into the telogen (resting) phase, leading to shedding. Some patients notice early thinning in just a few weeks, but sudden loss within hours or days does not occur because the hair growth cycle takes time to reflect systemic changes.
Most cases of lamotrigine-related alopecia were reported in the first few months of therapy and often improved after dose reduction or discontinuation according to “Alopecia in Association with Lamotrigine Use: An Analysis of Individual Case Safety Reports in a Global Database” (Drug Safety, 2010).
How Does Lamotrigine Disrupt the Normal Hair Growth Cycle?
Lamotrigine disrupts the normal hair growth cycle by triggering telogen effluvium, a condition where a higher proportion of follicles prematurely shift from the active growth (anagen) phase into the resting (telogen) phase, leading to diffuse shedding. This disruption likely results from drug-induced stress responses, hormonal alterations, or interference with cellular energy metabolism in follicular keratinocytes.
Over time, the shortened anagen phase and increased telogen activity reduce visible density, although regrowth is usually possible if follicles remain structurally intact. Patients often notice thinning 2–6 months after initiating therapy, aligning with the delayed cycle turnover of scalp hair.
How Does Depression-Induced Cortisol Elevation Affect Hair Follicles?
Depression elevates cortisol, the body’s primary stress hormone, which directly weakens hair follicles by shortening the anagen (growth) phase and pushing more hairs into the telogen (resting) phase, leading to diffuse thinning and increased shedding. Chronically high cortisol levels constrict blood vessels, reducing oxygen and nutrient delivery to the scalp, and increase local inflammation that damages follicular stem cells.
This mechanism explains why people with major depressive disorder often present with telogen effluvium and fragile hair texture. Elevated cortisol disrupts normal follicle cycling and accelerates aging-like processes in the scalp.
Depressed patients had significantly higher cortisol accumulation in scalp hair samples, correlating with hair loss severity as “Hair Cortisol Concentrations as a Biomarker of Chronic Stress in Patients with Depression” (Psychoneuroendocrinology, 2017) showed.
Unlike blood tests that only reflect momentary hormone levels, hair cortisol analysis reveals chronic systemic stress over months, making the hair strand itself a living “stress diary.” This means the very hair being lost already carries biochemical evidence of the hair loss due to depression. We describe this phenomenon as “emotion memory in hair”; the idea that hair itself records the body’s emotional and hormonal history, carrying molecular traces of stress, trauma, or imbalance that can explain patterns of hair loss linked to depression.
When Does Telogen Effluvium Hair Loss Typically Begin After Starting Lamotrigine?
Telogen effluvium hair loss typically begins within 2–3 months after starting lamotrigine, as the medication pushes a higher number of follicles into the resting (telogen) phase prematurely. This delay reflects the normal biology of hair cycling, where shedding occurs only after the telogen phase completes and hairs detach from the scalp.
Lamotrigine’s characteristics that trigger telogen effluvium include its effect on follicular metabolism, stress responses, and possible hormonal shifts in vulnerable patients. While not universal, this mechanism explains why shedding appears weeks to months after therapy initiation rather than immediately.
Why Might Epilepsy Patients Be More Susceptible to Hair Loss from Lamotrigine?
Epilepsy patients are more susceptible to hair loss from lamotrigine because they often take the drug long-term and sometimes in combination with other antiseizure medications, which increases the cumulative risk of adverse effects including alopecia. In these patients, the stress of recurrent seizures, nutritional deficiencies, and polytherapy amplifies vulnerability to epilepsy hair loss, making them more likely to report thinning or shedding compared to other groups.
Chronic epilepsy itself is associated with systemic metabolic stress and oxidative imbalance, both of which weaken follicular health. This overlap means that distinguishing between epilepsy and hair loss as a disease-related issue versus a lamotrigine-induced side effect is clinically challenging.
Alopecia was more frequently reported in epilepsy patients taking lamotrigine compared to individuals using the drug for psychiatric disorders according to “Antiseizure Medication-Induced Alopecia: A Literature Review” (Brain Sciences, 2023), underscoring the role of comorbidities and polytherapy in raising susceptibility.
How Does Mood Instability in Bipolar Disorder Impact Hair Follicle Health?
Mood instability in bipolar disorder negatively impacts hair follicle health for some patients by overactivating the body’s stress response system, disrupting hormonal balance, and fueling chronic inflammation. Patients with bipolar disorder often experience elevated cortisol due to repeated mood swings, and this heightened stress hormone directly interferes with the hair cycle, pushing follicles into the telogen (resting) phase and increasing shedding.
Chronic dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis reduces scalp blood flow and impairs nutrient delivery, leaving follicles vulnerable to miniaturization and thinning. The oxidative stress linked to bipolar mood episodes amplifies inflammatory cytokine activity in the skin, weakening follicle stem cells over time. These mechanisms explain why bipolar hair loss persists even in patients not taking hair-loss–associated medications.
The hypothalamic-pituitary-adrenal (HPA) axis is your body’s main stress-response system. It works like a chain of command:
- The hypothalamus in your brain senses stress.
- It signals the pituitary gland, which then tells the adrenal glands to release stress hormones like cortisol.
Chronic dysregulation means that this system is overactive or misfiring for long periods; which often happens in people with bipolar disorder due to repeated mood swings and stress episodes.
Now, why does this matter for hair?
- When cortisol levels stay high, blood vessels in the scalp narrow (called vasoconstriction).
- Narrowed blood vessels = less blood flow to hair follicles.
- Less blood flow = reduced delivery of oxygen and nutrients that follicles need to grow strong, healthy hair.
- Over time, the deprived follicles miniaturize (shrink), producing thinner and weaker hairs, which eventually fall out.
too much stress hormone from an unstable HPA axis “starves” the follicles, making them shrink and shed hair.
Mood-related cortisol surges impair keratinocyte proliferation and alter hair follicle cycling, reinforcing the connection between bipolar disorder and hair loss beyond drug side effects according to “Psychological Stress and Hair Loss: Possible Mechanisms” (Experimental Dermatology, 2017)
What Does Hair Look Like Before and After Lamotrigine Hair Loss?
Do an image carousel at the end of the statement for different pictures of hair before and after having a Lamotrigine hair loss with Image Alt Tags
Before lamotrigine-related hair loss, most patients report normal scalp coverage with stable density, while after developing lamotrigine side effects hair loss, the hair often appears diffusely thinned, brittle, and lacking volume.
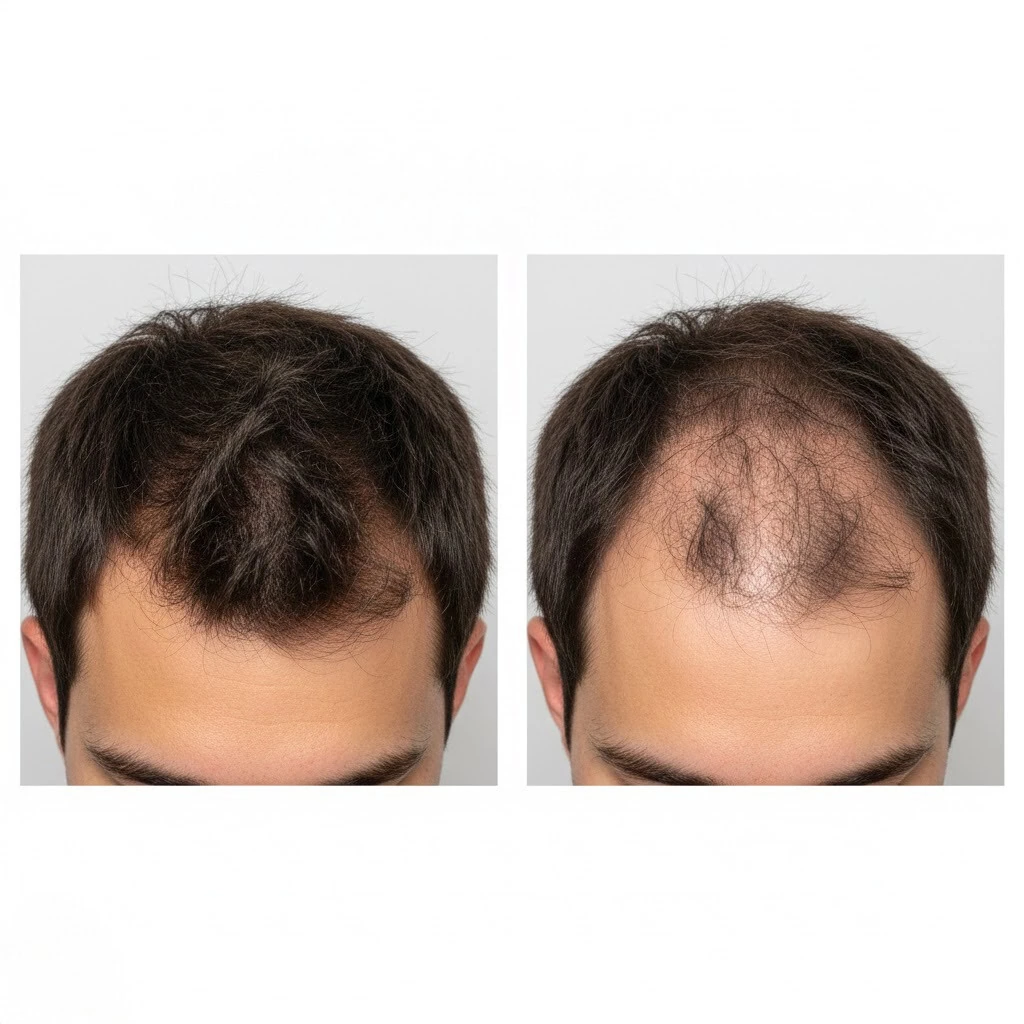
In some cases, shedding follows the pattern of telogen effluvium, with widespread thinning across the scalp, while others experience patchier hair density depending on follicular sensitivity. These changes are usually reversible after dose adjustment or discontinuation, though recovery takes several months as follicles re-enter the growth cycle.
How to Stop Hair Loss from Lamotrigine
Stopping lamotrigine hair loss involves reviewing the medication plan with a doctor and combining supportive therapies that protect follicle health and restore the growth cycle.
- Medical Dose Adjustment: Lowering or discontinuing lamotrigine under medical supervision often improves hair shedding. Many patients reported regrowth within months according to Drug Safety (2010).
- Switching to Alternative Therapy: If alopecia persists, psychiatrists prescribe another mood stabilizer with a lower risk of hair loss. This is needed when quality of life is affected by ongoing shedding.
- Nutritional Support: Supplementing with zinc, iron, folate, B vitamins, and biotin helps counter nutrient-related disruptions. Hair thickness usually begins to improve in 3–6 months if deficiencies are corrected.
- Topical Scalp Treatments: Minoxidil and similar agents extend the anagen (growth) phase, supporting faster regrowth. Results often appear after 4–6 months of consistent use.
- Lifestyle and Scalp Care: Stress management, gentle hair care routines, and avoiding harsh shampoos or chemicals prevent further weakening of follicles during recovery.
- Hair Transplant (Last Resort): For patients with permanent thinning after lamotrigine, a hair transplant becomes an option. This is only recommended after at least 12–18 months, once medication-related shedding has stabilized.
Most cases of lamotrigine-related hair loss are reversible, with regrowth starting in 3–6 months and full recovery possible within 12 months, provided the drug is adjusted and supportive care is in place.
How Effective Is a Hair Transplant for Lamotrigine-Induced Permanent Hair Loss?
A hair transplant is an effective solution for lamotrigine-induced permanent hair loss, particularly when follicles have been irreversibly damaged and no longer recover after medication adjustment. While most cases of lamotrigine hair loss improve within 3–12 months after dose reduction or discontinuation, a subset of patients experience lasting thinning that only surgical restoration corrects.
Hair transplants are usually recommended after at least 12–18 months, once medication-related shedding has stabilized and the scalp’s natural regrowth potential is fully assessed. This prevents unnecessary surgery during temporary telogen effluvium phases and ensures that only true permanent loss is treated.
Patients who choose hair transplants in Turkey benefit from internationally recognized expertise, advanced techniques like FUE and DHI, and competitive pricing that makes large sessions more affordable compared to Europe or the United States.
Among leading providers, Vera Clinic is widely regarded as the best hair transplant clinic in Turkey, known for combining scientific excellence with innovative methods such as Oxycure Therapy to maximize graft survival and long-term density.
What to Expect Before and After a Hair Transplant for Lamotrigine Hair Loss?
Before the Transplant: Your surgeon confirms that lamotrigine-related shedding has stabilized, maps graft counts, and preps the donor/recipient sites for natural density and direction.
After the Transplant: Expect temporary shedding in 2–4 weeks, visible regrowth from 3–4 months, and fuller coverage by 9–12 months as grafts cycle into anagen.
Check the lamotrigine hair transplant before and after results at Vera Clinic below!
When to See a Dermatologist for Hair Loss due to Lamotrigine
You should see a dermatologist if lamotrigine hair loss is rapid, persistent beyond three months, or accompanied by severe symptoms such as scalp pain, patchy bald spots, visible inflammation, or signs of infection like oozing and crusting.
In cases where thinning does not reverse after stopping the drug, a hair transplant consultation is recommended to evaluate permanent loss and possible surgical restoration.
How is Lamotrigine Hair Loss Diagnosed?
Lamotrigine hair loss is diagnosed through a detailed medication history, clinical scalp examination, and ruling out other causes such as thyroid dysfunction or nutritional deficiencies.
Which Antidepressants Are Less Likely to Cause Hair Loss?
Some antidepressants are less frequently associated with hair loss compared to others, and patients often tolerate them better in terms of scalp health.
- SSRIs (Selective Serotonin Reuptake Inhibitors): SSRIs such as sertraline and escitalopram are rarely linked to alopecia. When hair shedding does occur, it is usually mild and reversible after dose adjustment. A retrospective review in Journal of Clinical Psychopharmacology (2018) found that SSRIs had significantly lower reports of hair loss compared to bupropion and tricyclic antidepressants.
- SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors): Duloxetine and venlafaxine show lower rates of hair loss compared to other drug classes. In a Pharmacoepidemiology and Drug Safety (2019) analysis of FDA adverse event data, SNRIs were less represented in alopecia reports compared with bupropion and mood stabilizers like lamotrigine.
- Mirtazapine: This atypical antidepressant is often chosen when patients develop hair loss on SSRIs or SNRIs. Reports of mirtazapine-induced alopecia are exceedingly rare. A case series in Psychiatry Investigation (2015) noted hair regrowth after switching patients from fluoxetine to mirtazapine.
- Agomelatine: As a melatonergic antidepressant, agomelatine is distinct from SSRIs and SNRIs, and alopecia is not commonly reported in clinical trials. European Neuropsychopharmacology (2017) trial data reported no significant increase in hair loss versus placebo.
- Vilazodone and Vortioxetine: These newer multimodal antidepressants have fewer long-term side effects, including alopecia. Adverse event monitoring in CNS Drugs (2020) noted very low incidence of reported hair loss with both agents.
A 2021 review in Annals of Clinical Psychiatry emphasized that bupropion carries the highest risk of antidepressant-related hair loss, whereas SSRIs and SNRIs remain the safest List of Antidepressants that Cause Hair Loss class overall for patients concerned with alopecia.
Which Other Types of SARI Antidepressants can Cause Hair Loss?
SARI (Serotonin Antagonist and Reuptake Inhibitor) antidepressants aside from lamotrigine have been linked to alopecia in clinical observations, though the risk differs by compound and dosage.
- Trazodone: Trazodone is primarily used for depression and insomnia. Hair loss cases are rare but documented, usually presenting as telogen effluvium. Unlike lamotrigine hair loss, trazodone-induced shedding often resolves after discontinuation. A pharmacovigilance report in Journal of Clinical Psychopharmacology (2016) highlighted trazodone among antidepressants occasionally associated with alopecia.
- Nefazodone: Nefazodone, though less commonly prescribed today due to liver toxicity concerns, has been reported in isolated cases to cause diffuse hair thinning. The mechanism appears related to serotonin receptor modulation and metabolic stress on follicles. Compared to lamotrigine, nefazodone-related alopecia is less studied but has been noted in Drug Safety Reports (2004).
- Etoperidone: Etoperidone, an older SARI not widely available, has shown occasional associations with scalp hair shedding. Its serotonergic and adrenergic interactions disrupt follicle cycling in sensitive patients, though the data are limited.
While lamotrigine hair loss is often studied in the context of anticonvulsants and mood stabilizers, other SARIs like trazodone and nefazodone have been linked to alopecia.
The difference lies in the mechanism: lamotrigine is associated with metabolic and follicular cycle disruption, while SARIs like trazodone more often trigger telogen effluvium due to serotonin-driven scalp inflammation.
Does Changing Antidepressants Reverse Hair Loss Caused by Lamotrigine?
Yes. In many patients, switching from lamotrigine to another antidepressant leads to gradual reversal of hair loss, particularly when the shedding is due to telogen effluvium rather than permanent follicle damage. A large proportion of patients experiencing lamotrigine side effects hair loss improved after either lowering the dose or transitioning to a different antidepressant.
However, regrowth is not immediate; most patients begin to notice improvement after 3–6 months, as the hair follicles cycle back into anagen (growth phase). In rare cases where follicular scarring or long-term anagen effluvium has occurred, hair loss is only partially reversible, and surgical options like a hair transplant is required.
How to Prevent Hair Loss when Taking Lamotrigine
Hair shedding on lamotrigine is not inevitable, and careful preventive steps reduce the risk of follicle stress and improve recovery rates.
- Regular Dermatology Monitoring: Schedule early scalp check-ups to detect telogen effluvium or anagen effluvium before they progress. A dermatologist differentiates between temporary shedding and drug-induced follicle toxicity.
- Nutritional Optimization: Maintain adequate levels of zinc, iron, biotin, and vitamin D, which are frequently deficient in patients on long-term anticonvulsant therapy. A review in Brain Sciences (2023) highlighted that correcting micronutrient deficiencies improved hair regrowth in several lamotrigine-associated alopecia cases.
- Dose Adjustments: Work with your physician to review dosing. The 2010 Drug Safety analysis of 337 lamotrigine hair loss cases showed many patients experienced regrowth after dose reduction without discontinuing the drug entirely.
- Stress and Cortisol Management: Since mood disorders and medication stress both elevate cortisol, integrate stress-reduction strategies (e.g., mindfulness, CBT, or yoga) to prevent HPA axis dysregulation, which has been linked to follicle miniaturization.
- Topical and Supportive Therapies: Minoxidil or PRP (platelet-rich plasma) support follicular activity during drug-induced shedding. These therapies help shorten the telogen resting phase and accelerate anagen regrowth.
- Switching Antidepressants if Needed: If hair loss persists beyond six months, a medication review with your psychiatrist is warranted. Many patients regain density after transitioning from lamotrigine to lower-risk agents such as SSRIs (sertraline, escitalopram).