Lupus Hair Loss happens when the body does not get the nutrients it needs to sustain good hair growth, and is a cause of lupus hair loss. The maintenance of the hair growth cycle depends on vital nutrients (protein, iron, zinc, biotin, and vitamins A, D, and E). The body prioritizes necessary organ function over non-essential processes like hair creation when the nutrients are deficient, which results in hair thinning, shedding, and, in extreme situations, bald patches. Increased hair loss while brushing or washing, brittle, dry strands, and scattered thinning across the scalp are indicators of malnutrition-related hair loss. Treatments aim to address the underlying vitamin deficiencies through a well-balanced diet, tailored supplements, and medical care.
Lupus hair loss is defined as hair shedding and thinning caused by lupus, a chronic inflammatory disease in which the immune system mistakenly attacks healthy tissues such as the skin and hair follicles. The immunological response disrupts the natural hair growth cycle, resulting in excessive shedding or permanent scarring hair loss. Lupus symptoms are related to inflammation and damage to hair follicles, resulting in temporary or permanent hair loss. Lupus-related hair loss is classified as scarring and non-scarring alopecia. Lupus hair loss that does not leave scars is characterized by diffuse thinning or increased shedding and is treatable. Scarring alopecia is known as discoid lupus erythematosus (DLE), which damages hair follicles, leading to irreparable bald patches if not treated immediately.
Lupus-related hair loss is caused by inflammation of the scalp, discoid lupus lesions, stress from disease flare-ups, lupus drugs, or nutritional inadequacies. Lupus induces skin inflammation on the scalp, triggering follicle damage and hair shedding. Scarring and irreversible hair loss result from discoid lupus symptoms, which include elevated, scaly, and inflamed regions on the scalp. Lupus flare-ups produce physical stress on the body, which leads to a transient kind of hair loss (telogen effluvium) in which hair prematurely starts the shedding phase. Immunosuppressants, corticosteroids, and other lupus hair loss treatments are recommended by dermatologists. Lupus patients develop malabsorption or appetite loss.
What Is Lupus Hair Loss?
Lupus hair loss results from autoimmune attacks on skin and hair follicles. Discoid Lupus Erythematosus (DLE) is a chronic form that causes red, inflamed, scaly scalp lesions, damaging hair follicles through inflammation, leading to permanent scarring and hair loss if untreated. Lupus affects the body by triggering inflammatory responses, damaging organs and tissues (skin, joints, kidneys, and hair follicles). The immune attack triggers inflammation around the hair follicles when lupus targets the scalp, disrupting the normal hair growth cycle and causing excessive hair shedding. The autoimmune response pushes hair follicles into the resting (telogen) phase, leading to telogen effluvium, where large amounts of hair are shed at once.
Lupus alopecia appears as temporary (non-scarring hair loss) and improves with proper treatment, and permanent hair loss (scarring alopecia). The discoid lupus hair loss is an exception to hair transplantation because of its severity. Taking care of lupus-related hair loss means working together with the healthcare team to manage symptoms and explore different treatment options to feel better and more confident. The autoimmune disease that causes hair loss and inflammation is treated with medications such as corticosteroids, immunosuppressants, and antimalarial drugs. Getting diagnosed early and starting treatment makes a positive difference. Patients feel better and prevent serious problems from developing later on down the line.
Is hair loss a sign of lupus?
Yes, hair loss is a sign of lupus because the body’s immune system mistakenly harms healthy tissues in the skin and hair follicles. Systemic lupus erythematosus (SLE) and cutaneous lupus erythematosus (CLE) lead to hair loss. The immune reaction causes the scalp to become inflamed, leading to uneven, diffuse bald patches or, in more extreme situations, alopecia that leaves permanent scars. Large volumes of hair come out during ordinary activities (brushing or washing), a condition (telogen effluvium), which is brought on by lupus flares, which are episodes of the disease.
Discoid lesions are a type of skin rash associated with lupus, harming hair follicles and causing irreversible damage if treatment is not given. Stress, malnutrition, and adverse reactions to drugs (immunosuppressants or corticosteroids) used to treat lupus are other contributing factors. Rapid or unusual hair loss, when accompanied by other lupus symptoms, such as fatigue, joint pain, skin rashes, or photosensitivity, triggers a medical examination for lupus or flare-ups.
How Does Lupus Cause Hair Loss?
Lupus causes hair loss through the body’s autoimmune and inflammatory responses that target healthy skin and hair follicles. A chronic autoimmune disease, lupus damages the body’s tissues by causing the immune system to attack them mistakenly. The question, “Does lupus make your hair fall out?” is asked by patients who have no idea about their disorders. The scalp suffers from the attack, causing follicle damage and interfering with the body’s natural hair growth cycle. Lupus leads to hair loss, influenced by how severe and what type it is. The common inflammation-related condition (telogen effluvium) happens when hair follicles prematurely enter the resting (shedding) phase during lupus, leading to hair thinning flare-ups.
The results in sudden, widespread hair shedding across the scalp. The severe form of lupus and hair loss is Discoid Lupus Erythematosus (DLE), which causes red, inflamed lesions on the scalp that leave scars on the hair follicles. The discoid lupus erythematosus hair loss occurs in the disease. Patients notice more hair falling out during flare-ups, while others develop bald patches because of persistent scalp inflammation or the side effects of medications (corticosteroids and immunosuppressants).
How does lupus cause sores and lesions?
Lupus causes sores and lesions through the autoimmune response that triggers inflammation in the skin layers, leading to raised, scaly, and red patches. Lesions show up on the scalp and bother the hair follicles, which causes hair to fall out. Lupus-related hair loss occurs because of a combination of immune system challenges, inflammation, and side effects from medications.
Where on the Scalp Does Hair Loss Typically Occur with Lupus?
Lupus-related hair loss occurs in areas of the scalp where inflammation and lesions form, such as the crown, sides, and frontal hairline. Discoid Lupus Erythematosus (DLE) is a skin-related variant of lupus that causes a lupus hair loss pattern in regions affected by the characteristic red, inflammatory, and scaly lesions. Lesions appear anywhere on the scalp, but they start on the crown or top of the head, areas that are exposed to environmental factors like UV light. The affected areas in “early discoid lupus scalp” enlarge as the disease worsens, resulting in patchy bald spots or large patches of hair loss thinning, according to “Scarring alopecia in discoid lupus erythematosus” (C.L. Wilson, S.M. Burge, 1992). Hair loss in non-scarring lupus alopecia shows noticeable thinning throughout the entire scalp, rather than in isolated patches during lupus flare-ups that cause a condition in which many hair follicles start the shedding phase prematurely (telogen effluvium). The vertex and frontal scalp regions are impacted in lupus-related alopecia. The areas in “discoid lupus erythematosus scalp” are exposed to environmental stressors and triggers.
Does Lupus Always Lead to Hair Thinning?
No, lupus does not always lead to hair thinning, but it is a common symptom observed by persons with the condition during disease flares. Lupus hair loss is caused by the body’s autoimmune reaction, in which the immune system unintentionally assaults healthy tissues. The immunological activity causes inflammation surrounding the follicles, disrupting the normal hair growth cycle and forcing many hairs into the resting (telogen) phase, resulting in profuse shedding and visible thinning over the scalp. The degree and frequency of hair loss are determined by the kind of lupus, the level of disease activity, and the condition’s management.
Hair thinning in systemic lupus erythematosus (SLE) is diffuse and transitory, and it improves once the disease is under control or the inflammation goes down. Discoid Lupus Erythematosus (DLE) patients experience more permanent and localized hair loss as a result of scarring. The timely medication intended to reduce inflammation and immune system activity, lupus hair thinning is repaired, according to a study “International Journal of Dermatology” (2019). They showed that over 45% of individuals with systemic lupus experience diffuse thinning at times when the disease is active.
How Common Is Hair Loss from Lupus?
Lupus-related hair loss is a common symptom affecting a large proportion of patients who are diagnosed with the disease. Research indicates that between 45 and 55 percent of patients with systemic lupus erythematosus (SLE) lose some hair while they are unwell. Lupus-related hair loss occurs in women compared to men. Pregnant women are prone to developing the disease in over 90% of lupus cases. Hormonal factors (estrogen swings and a stronger immunity) in thinning “women’s lupus hairline” are thought to be related to the higher prevalence of lupus and the increased risk of associated hair loss.
Discoid Lupus Erythematosus (DLE) is common in women and is a type of lupus that causes scarring and irreversible hair loss. The combination of hormonal variables and a genetic tendency that predisposes women to autoimmune illnesses causes it. Adults aged 11 to 45 are the age group most affected, with women in their 20s to 40s having the highest statistics. Children and older adults develop lupus, but it is less common. Female lupus hair loss affects up to 85% of patients with lupus, and it becomes common in women, who compose 93% of lupus cases in Turkey. The incidence of “lupus symptoms women” ranges from 4.4 to 4.8 per 100,000 population per year, with an average rate of 52 per 100,000 (98 in women vs. 7 in men).
What Does Hair Loss from Lupus Look Like on the Scalp?
Hair loss from lupus on the scalp looks dry, fragile, and brittle, making it prone to breaking easily. Lupus-related hair loss (lupus alopecia) is present on the scalp, based on the type and severity of the disorder. Diffuse thinning, where the hair appears thinner across the entire scalp (the frontal hairline and crown), characterizes physical features. It occurs during flare-ups of lupus, when inflammation disrupts the hair development cycle and causes profuse shedding.
Discoid Lupus Erythematosus (DLE) causes hair loss, round or oval bald patches. The patches are associated with apparent skin abnormalities on the scalp (redness, scaling, and discoloration). Scarring forms in the damaged areas, leaving the scalp smooth and glossy despite the irreversible loss of hair follicles. Lupus hair loss varies from mild diffuse thinning to severe, patchy baldness with irritated or scarred skin, making early diagnosis and treatment crucial to prevent permanent damage. Patients and medical professionals distinguish between permanent, scarring alopecia and temporary, reversible lupus hair loss by looking at lupus hair loss photos.
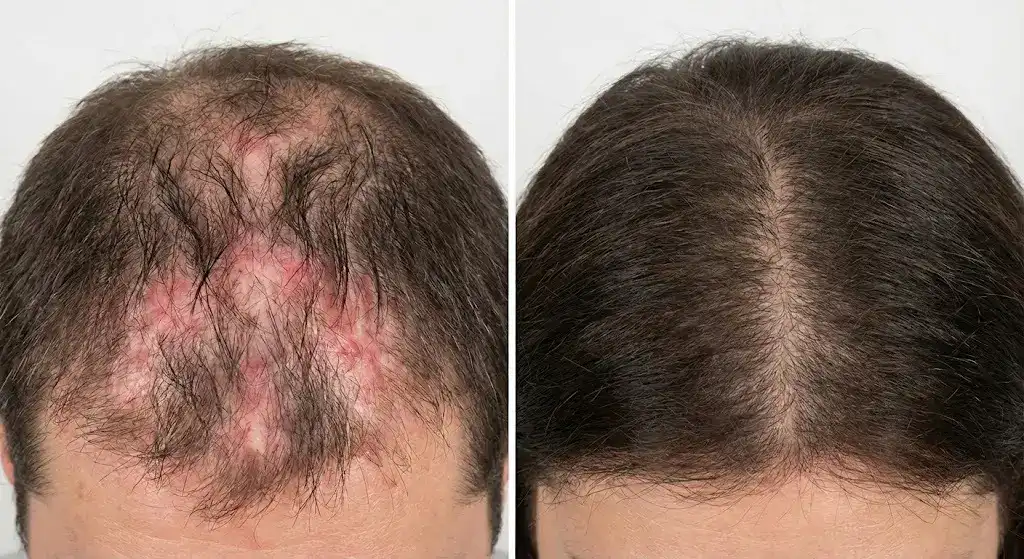
What Does Hair Look Like Before and After Having Lupus Hair Loss?
Hair looks like before and after having lupus hair loss varies from full (thick) to bald. Patients have full, healthy hair distributed across their scalp before they start to lose it due to lupus. The person’s hair texture is normal, whether straight, wavy, or curly, with no noticeable thinning or patchiness. The scalp seems smooth and devoid of scaling, blemishes, or redness. Changes in the hair and scalp become apparent once lupus hair loss starts.
The hair begins to appear thinner around the frontal hairline, temples, and crown. Patients notice an increase in hair shedding while brushing or washing. Lupus develops distinct bald patches with noticeable scalp inflammation, such as redness, flakiness, or scaly lesions. The hair becomes brittle, dry, and prone to breaking, which results in uneven texture and length.
Discoid Lupus Erythematosus (DLE) patients exhibit long-lasting scarring. The areas appear smooth, shiny, and lack hair follicles, leading to irreversible bald spots if left untreated. Non-scarring lupus-related hair loss recovers with good medication and illness control, allowing hair to sprout and the scalp to regain a healthy appearance.
What Are the Lupus Hair Loss Symptoms?
The lupus hair loss symptoms are categorized into mild, severe, and rare forms, depending on the type of lupus, disease activity, and individual response. Common symptoms include diffuse hair loss across the scalp and increased daily hair shedding, which is noticeable when brushing or shampooing. The hair becomes dry, brittle, and prone to breaking. A patient experiences “lupus hairs,” which are short, broken strands that appear close to the temples and frontal hairline.
Discoid Lupus Erythematosus (DLE) is a condition where lupus causes severe signs of hair loss. The disorder causes red, scaly, and irritated patches on the scalp, which destroy hair follicles. The lesions cause scarring alopecia, which leaves smooth, glossy bald areas where hair never comes back, if treatment is not received.
Rare lupus symptoms like patchy hair loss outside the scalp (eyebrows, eyelashes, or body hair) occur during severe systemic lupus flare-ups. Patients have telogen effluvium, an uncommon but widespread loss of hair induced by the physical stress of lupus or its treatment. A rare symptom of lupus is hair loss that signals underlying autoimmune and inflammatory activity in the body, and early detection and treatment are essential for reducing long-term hair loss damage.
What Are the Common Symptoms of Lupus Hair Loss?
Common symptoms of lupus hair loss are listed below.
- Discoid Lupus Erythematosus (DLE): Scarring caused by red, inflammatory lesions on the scalp and other areas of the skin that bear hair. DLE results in permanent hair loss, according to an article “Is Your Hair Loss Due to Lupus?” (Rheumatology Center of New Jersey).
- Telogen Effluvium: Hair falls out in clumps or sudden heavy hair loss (telogen effluvium), a sign of chronic inflammation, and usually non-scarring and reversible once the flare is under control.
- Hairs in Other Body Parts: Body hair loss happens during periods of acute disease activity. Lupus causes extensive immune system attacks on hair follicles, leading to loss of hair on the scalp, eyebrows, eyelashes, beard, and other body parts.
- Existing Diseases: Lupus-related signs that appear with hair loss are chronic fatigue, joint pain, skin rashes, and kidney disease. The presence of multiple signs shows an active lupus flare, in which the body’s immune system is attacking the skin and hair follicles.
Common lupus symptoms vary depending on age, gender, demographic background, genetic makeup, and underlying health issues. Lupus is aggressive in childhood, but lupus in adulthood is milder but dangerous. Demographic characteristics affect the appearance and severity. The socioeconomic situation has an impact on disease management and flare severity. A family history of lupus or other autoimmune disorders raises the risk, so genetics plays a part. The pre-existing medical disorders worsen symptoms and make diagnosis and treatment challenging.
When Does a Scalp Rash Occur in Lupus Patients?
A scalp rash occurs in lupus patients when the autoimmune condition affects the skin in the form of Discoid Lupus Erythematosus (DLE) or Acute Cutaneous Lupus Erythematosus (ACLE). Lupus flares, periods of increased disease activity, trigger a scalp rash. DLE presents as round, scaly, red, or raised patches on the scalp that lead to scarring and hair loss over time. ACLE causes a broader rash, including the scalp, during systemic flare-ups.
Lupus is an autoimmune disorder in which the body’s immune system mistakenly attacks healthy skin cells. It causes red, thick, scaly plaques to form (localized inflammation), burning or itching, and damage to hair follicles when on the scalp. Discoid lupus lesions impact the scalp, creating patches that consolidate into scarring alopecia if left untreated. Scalp rashes in lupus emerge during disease flare, cutaneous (DLE and ACLE) through autoimmune-linked inflammation that damages skin and hair follicles, leading to permanent hair loss, according to “StatPearls: Discoid Lupus Erythematosus” (Brianna McDaniel; Sukesh Sukumaran; Thoyaja Koritala; Laura S. Tanner, 2023).
What Are the Severe Symptoms of Lupus Hair Loss?
Severe symptoms of lupus hair loss are listed below.
- Non-Scarring Alopecia: The diffuse, severe non-scarring alopecia with significant scalp thinning. Trichoscopy shows signs like arborizing blood vessels, black dots, and hypopigmented thin hairs, indicating active, severe disease, according to “Hair Disorders in Autoimmune Diseases” (Giselle Rodríguez-Tamez et al., 2023).
- Patchy Baldness: Non-scarring alopecia around 14.8% of patients, who experienced distinct patches of hair loss, and 15.1% noticed new patches after their diagnosis. Severe patches lead to complete hair loss in small areas, which is mistaken for alopecia areata if trichoscopy is not used for evaluation.
- Lupus Hairs: Lupus hair (frontal hairline breakage) affects 5% to 30% of chronic active systemic lupus erythematosus patients, characterized as fragile, short “lupus hairs” at the anterior hairline, with breakage and slow regrowth.
- Scarring Alopecia: Scarring (Cicatricial) alopecia or discoid lesions occur when discoid lupus lesions damage hair follicles, leading to permanent coin-shaped bald spots, scaly plaques characteristic of chronic cutaneous lupus erythematosus.
- Clumps of Hair: Clumping and sudden shedding are known in severe flares. A hair-pull test is positive in diffuse, patchy, and lupus‑hair types.
- Severe Body Hair Loss: Extra-scalp hair loss beyond the scalp, lupus causes eyebrow, eyelash, beard, and body hair loss in severe cases.
- Systemic Disease: Correlation with systemic disease activity, severe diffuse hair loss correlates with systemic involvement: blood abnormalities and renal involvement are seen in trichoscopic findings.
Severe lupus symptoms, including permanent scarring alopecia, diffuse hair loss, and painful scalp lesions, are influenced by age, gender, demographics, genetics, and underlying health conditions. Childhood-onset lupus is aggressive, while older adults are prone to treatment-related hair loss. Gender differences are observed, with African American, Hispanic, and Asian patients facing severe cutaneous lupus and scarring alopecia. The genetic factors, underlying health conditions, and medications contribute to the severity and progression of lupus symptoms.
What Are the Rare Symptoms of Lupus Hair Loss?
Rare symptoms of lupus hair loss are listed below.
- Cutaneous Lupus Erythematosus: A less common subtype of chronic cutaneous lupus that mimics alopecia areata. The lesions appear as non-scarring, urticarial-like papules or plaques and cause patchy hair loss on sun-exposed scalp areas. Diagnosis requires biopsy, revealing dense dermal lymphocytic infiltrate with increased mucin. Treated effectively with antimalarials, according to “Areata-Like Lupus as a Clinical Manifestation of Cutaneous Lupus Erythematosus” (Karina Lopes Morais et al., 2022).
- Lupus-Specific Disease: Areata‑like lupus alopecia is a form of non-scarring patchy hair loss that resembles alopecia areata, including trichoscopic signs like “exclamation‑mark” hairs. Histology shows lupus-specific interface dermatitis and immune complex deposits, helping differentiate it from classic alopecia areata.
- Linear and Annular Lupus Panniculitis of the Scalp (LALPS): Hair loss is present as linear or ring-shaped non-scarring alopecia following Blaschko’s lines, common in young Asian males. Histopathology shows deep subcutaneous inflammation, sparing hair follicle stem cells, making it reversible with treatment.
- Frontal Fibrosing Alopecia (FFA): Overlap with FFA are rare cases reporting the co-occurrence of lupus (discoid or systemic) with frontal fibrosing alopecia, a scarring form affecting the front hairline and eyebrows. Biopsies reveal features of conditions.
- Anagen Effluvium: The anagen effluvium is due to lupus or its treatments. Rapid hair loss arising within days of initiating cytotoxic lupus treatments (cyclophosphamide, methotrexate) or severe systemic flare, characterized by dystrophic anagen hairs and scalp shedding.
Rare lupus symptoms are influenced by age, gender, demographics, genetic factors, and underlying health conditions, which affect hair loss patterns. Younger patients, Asian males, are prone to experience LALPS, while older adults encounter diffuse hair loss or medication-induced hair loss. Ethnicity and demographics affect presentation, with Asian and Hispanic populations having higher rates of severe cutaneous lupus forms. Genetic predisposition, underlying health conditions, and immunosuppressive treatments contribute to the individualized appearance and severity of the symptoms.
How Do You Know If You Have Lupus Hair Loss?
You know if you have lupus hair loss by the symptoms listed below.
- Clinical Scalp Examination and History: Examine the scalp and hair, identifying patterns of loss (diffuse, patchy, “lupus hair”), the appearance of scaly plaques, scars, or broken strands. Dermatologists examine the scalp for erythema, scaling, and follicular clogging (“carpet-tack”), and sun sensitivity, flares, and medication history, according to “Nonscarring alopecia in systemic lupus erythematosus: A cross-sectional study with trichoscopic, histopathologic, and immunopathologic analyses” (Kumutnart Chanprapaph et al., 2019). Patients with diffuse thinning, patches, or brittle frontal hairs must be evaluated first. Lupus hair and scarring plaques along the frontal hairline are SLE features.
- Hair Pull or Tug Test: A manual examination in which 40 to 60 hairs are gently pulled. More than 10 hairs are found during the test, which is positive. Gently tug over multiple scalp locations, count the extracted hairs, and inspect them under a microscope to determine the kind of root (telogen vs. dystrophic anagen). Active shedding is indicated, which allows for the distinguishing of diffuse lupus alopecia from telogen effluvium. Widely used, but abnormal in lupus alopecia.
- Trichoscopy (Dermatoscopic Scalp Imaging): A non-invasive, magnified scalp exam that evaluates follicular and vascular patterns. A handheld or video dermoscope shows arborizing vessels, black spots, broken hairs, and follicular hyperkeratosis. Useful for identifying lupus-related loss from other alopecias and directing biopsy sites.
- Scalp Biopsy with Histopathology: A microscopic study of scalp tissue to detect lupus-related inflammation and scarring. A 4 mm punch biopsy, from the alopecic margin, is stained and examined for interface dermatitis, follicular destruction, and peri-follicular fibrosis. Required for distinguishing between scarring (discoid lupus) and non-scarring, or unusual patchy loss.
- Direct Immunofluorescence (DIF) on Scalp Tissue: Identifies immune complex deposition along basement membrane zones. A cryosection of the biopsy sample is stained with fluorescent antibodies. A granular accumulation pattern indicates lupus. Performed together with histology for a definite diagnosis in non-scarring cases. 78% of patients reported positive DIF at the dermoepidermal and follicular sites.
- Blood and Serologic Tests: Laboratory analysis of autoimmune markers and disease activity. Analyses include anti-double-stranded DNA (anti-dsDNA), complements (renal function, and urinalysis. Hair loss is associated with systemic lupus activity and is used to confirm it. Higher Systemic Lupus Erythematosus Disease Activity Index (SLEDAI) scores and proteinuria were connected to nonscarring alopecia in patients.
- Disease Activity Scoring: Standardized indices for assessing lupus activity and skin involvement. Clinical and analytical parameters are converted into numerical scores. Used to determine if hair loss correlates with chronic disease flare. SLEDAI score includes non-scarring alopecia, and disease activity correlates with hair alterations.
What Are the Lupus Hair Loss Treatments?
Lupus hair loss treatments are listed below.
- Topical and Intralesional Corticosteroids: Reduce inflammation at hair follicles. First-line treatment for cutaneous lupus to soothe the scalp lesions, according to “Treatment of Scarring Alopecia in Discoid Variant of Chronic Cutaneous Lupus Erythematosus With Tacrolimus Lotion, 0.3” (Emily C Milam, et al., 2015). Retrospective reports show significant lesion improvement and hair regrowth within 3 months in treatment-resistant cases using 0.3% tacrolimus lotion in combination with antimalarials and other therapies.
- Hydroxychloroquine: Systemic immunomodulator that lowers immune activity. Standard for controlling systemic and cutaneous disease. Discoid scalp lesions and regrowth with hydroxychloroquine and topical pimecrolimus. It takes about 3 to 6 months, but complete stabilization takes a bit longer. Regular maintenance for hair loss treatments or a new scalp influences the timeline of involvement.
- Oral Immunosuppressants: Suppress systemic inflammation to protect hair follicles. Patients with moderate-to-severe or steroid-resistant conditions need to undergo the treatment. The methotrexate, mycophenolate, and azathioprine are beneficial for resistant lupus alopecia, with 4 to 6 months to assess response.
- Janus-Associated Kinases Inhibitors (JAK): Blocks inflammatory cytokine signaling pathways. The diffuse, non-scarring alopecia occurs when conventional treatment fails. Hair regrowth after 4 weeks on tofacitinib, sustained at 8 months. Ruxolitinib resulted in full regrowth of hair in alopecia areata within 4 to 5 months. Severe, treatment-resistant, non-scarring types.
- Topical: Increases blood flow and prolongs the hair growth phase. It is valuable for thinning or non-scarring loss. Cited as helpful when combined with steroids or immunosuppressants. Topical minoxidil for telogen effluvium in lupus, in 3 to 6 months of regular use.
- Finasteride or Dutasteride: Inhibits a hormone linked to hair follicle shrinkage (DHT), for patients with androgenetic or mixed hair loss. Recommended with other lupus treatments for 6 to 12 months, but needs to be monitored for side effects.
- Platelet-Rich Plasma (PRP) Therapy: Concentrated growth factors promote follicular activity and help with non-scarring hair thinning. Systematic reviews indicate increased density with “3+ monthly injections”, three initial sessions followed by maintenance every 3 to 6 months.
- Low-Level Laser or LED Light Therapy (LLLT/LEDT): Stimulates follicle mitochondrial activity and circulation. Non-invasive methods encourage regrowth for alopecia areata. Hair density in 10 out of 11 trials for androgen and alopecia areata. Multiple sessions over 3 to 6 months are recommended.
- Nutritional Supplements and Support: Addresses deficiencies that worsen hair loss. Take iron, vitamin D, and biotin supplements if levels are low. Iron supplements are recommended for patients with anemia. Lupus patients benefit and vary based on nutritional status.
Hair transplants are an effective therapy option for lupus-related hair loss, but in cases when the disease is stable and no longer aggressive. Lupus activity must be well-controlled for at least 6 to 12 months before considering a transplant to avoid problems and ensure graft success. Dermatologists and rheumatologists prescribe hair transplants after establishing illness remission, because conducting the treatment during an active lupus flare results in poor healing and graft failure.
What Are the Best Shampoos for Lupus Hair Loss?
The best shampoos for lupus hair loss are listed below.
- Alpecin Caffeine Shampoo C1: Infused with caffeine, zinc, and niacin, the shampoo is designed to strengthen hair roots, penetrating follicles in just 2 minutes and prolonging the growth (anagen) phase. Lab and small clinical studies show improved hair strength and reduced shedding.
- Alpecin Hybrid Caffeine Shampoo: Similar to C1 and considered as the best shampoo for lupus hair loss, but with extra care ingredients for gentler cleansing on sensitive scalps. Offers the same caffeine benefits, making it safer for lupus-affected skin prone to dryness or irritation.
- First Botany Biotin & Stem‑Cell Hair Growth Shampoo: Combines with biotin, collagen, and plant stem cells to nourish hair shafts and support scalp health. Biotin and peptides strengthen hair, beneficial for lupus-related breakage, though caffeine’s circulation boost is missing here.
- Nioxin Hair Fall Defense Shampoo: Features caffeine, niacinamide, and lauric acid to stimulate scalp circulation and prevent breakage. Suitable for lupus patients seeking to protect shrinking hair follicles with added nourishment.
- Caffeine‑Infused Botanical Shampoo: A budget-friendly formula combining caffeine with salicylic acid and amino acids. Helps exfoliate scalp, boost circulation, and strengthen hair roots, ideal for mild lupus-related scalp discomfort.
- Gard Anti‑Hairfall Shampoo: Contains plant extracts common in Asian anti-hairfall products. Helpful in reinforcing hair strands, though it lacks the stronger stimulating effect of caffeine-based options.
How Effective Is Hair Transplant for Treating Hair Loss due to Lupus?
Hair transplant is effective for treating hair loss due to lupus if it is not related to a scarring condition. A hair transplant is a treatment for a condition caused by genetic hair loss or stable and well-managed lupus. Patients who have discoid lupus erythematosus (DLE) are not advised to undergo hair transplantation due to scarring that destroys hair follicles. Hair transplant must be considered if lupus is entirely and steadily under control and there are no visible symptoms of active inflammation on the scalp for at least 6 to 12 months. Performing surgery during an active flare results in low graft survival, increased scarring, and inadequate recovery.
Transplanting healthy hair follicles from places with dense hair (the back or sides of the head) to bald or thinning areas using Follicular Unit Extraction (FUE) or Follicular Unit Transplantation. The follicles develop a blood supply and start to produce new, natural-looking hair within a few months of being transplanted. Turkey is popular worldwide for providing low-cost, high-quality hair transplant treatments. Vera Clinic in Turkey has modern methods, highly qualified medical staff, individualized treatment programs, and affordable costs. Patients suffering from lupus-related permanent hair loss discover that an experienced Vera Clinic facility provides a secure and successful path to hair transplant and increased confidence.
What to Expect Before and After a Hair Transplant from Hair Loss due to Lupus
The expectations before and after a hair transplant for hair loss due to lupus are a complete medical examination and post-transplant care. Patients expect a full medical evaluation before getting a hair transplant for lupus-related hair loss to evaluate whether their lupus is well-controlled. Active lupus increases the risk of poor healing, graft failure, and scarring, which dermatologists and transplant surgeons require blood testing and scalp examinations to ensure the illness is stable. They recommend waiting until the last lupus flare before undergoing surgery. Doctors recommend treatments or changes to prescriptions to lessen inflammation and get the scalp ready for a successful transplant result.
The healing period following the transplant is longer than for patients without autoimmune disorders. Postoperative swelling, scabbing, and brief shedding of transplanted hairs (shock loss) are normal and subside slowly. New hair growth starts 3 to 4 months after the surgery, and full results are seen within 9 to 12 months. Slower regeneration or inadequate volume is at risk because lupus results in persistent swelling. Maintaining the best health and avoiding excessive hair loss in the surrounding areas requires careful post-transplant scalp care, continuous follow-up by the dermatologist, and regular lupus therapy. Understanding the requirements of hair transplant before and after care helps to achieve a fast recovery.
When to See a Dermatologist for Hair Loss due to Lupus
See a dermatologist for hair loss due to lupus when visible, patchy bald spots are accompanied by severe conditions of sudden shedding, and permanent scarring with irreversible hair loss (discoid lupus). Patients are experiencing scalp pain, inflammation, or blisters, joint pain, skin rashes, or exhaustion. A dermatologist is needed to see if a hair transplant consultation is an option. Early diagnosis and treatment prevent irreversible follicle damage and improve hair regeneration.